
- •Foreword I
- •Foreword II
- •Preface
- •Contents
- •1 Abscesses – Pyogenic Type
- •3 Cyst I – Typical Small
- •4 Cyst II – Typical Large with MR-CT Correlation
- •5 Cyst III – Multiple Small Lesions with MR-CT-US Comparison
- •6 Cyst IV – Adult Polycystic Liver Disease
- •7 Cystadenoma / Cystadenocarcinoma
- •8 Hemangioma I – Typical Small
- •10 Hemangioma III – Typical Giant
- •11 Hemangioma IV – Giant Type with a Large Central Scar
- •13 Hemangioma VI – Multiple with Perilesional Enhancement
- •14 Hemorrhage
- •16 Mucinous Metastasis – Mimicking an Hemangioma
- •17 Colorectal Metastases I – Typical Lesion
- •18 Colorectal Metastases II – Typical Multiple Lesions
- •19 Colorectal Metastases III – Metastasis Versus Cyst
- •20 Colorectal Metastases IV – Metastasis Versus Hemangiomas
- •21 Liver Metastases V – Large, Mucinous, Mimicking a Primary Liver Lesion
- •24 Breast Carcinoma Liver Metastases
- •25 Kahler’s Disease (Multiple Myeloma) Liver Metastases
- •26 Melanoma Liver Metastases I – Focal Type
- •27 Melanoma Liver Metastases II – Diffuse Type
- •28 Neuroendocrine Tumor I – Typical Liver Metastases
- •29 Neuroendocrine Tumor II – Pancreas Tumor Metastases
- •30 Neuroendocrine Tumor III – Gastrinoma Liver Metastases
- •31 Neuroendocrine Tumor IV – Carcinoid Tumor Liver Metastases
- •32 Neuroendocrine Tumor V – Peritoneal Spread
- •34 Renal Cell Carcinoma Liver Metastasis
- •35 Cirrhosis I – Liver Morphology
- •36 Cirrhosis II – Regenerative Nodules and Confluent Fibrosis
- •37 Cirrhosis III – Dysplastic Nodules
- •38 Cirrhosis IV – Dysplastic Nodules – HCC Transition
- •39 Cirrhosis V – Cyst in a Cirrhotic Liver
- •40 Cirrhosis VI – Multiple Cysts in a Cirrhotic Liver
- •41 Cirrhosis VII – Hemangioma in a Cirrhotic Liver
- •42 HCC in Cirrhosis I – Typical Small with Pathologic Correlation
- •43 HCC in Cirrhosis II – Small With and Without a Tumor Capsule
- •44 HCC in Cirrhosis III – Nodule-in-Nodule Appearance
- •45 HCC in Cirrhosis IV – Mosaic Pattern with Pathologic Correlation
- •47 HCC in Cirrhosis VI – Mosaic Pattern with Fatty Infiltration
- •48 HCC in Cirrhosis VII – Large Growing Lesion with Portal Invasion
- •49 HCC in Cirrhosis VIII – Segmental Diffuse with Portal Vein Thrombosis
- •50 HCC in Cirrhosis IX – Multiple Lesions Growing on Follow-up
- •51 HCC in Cirrhosis X – Capsular Retraction and Suspected Diaphragm Invasion
- •52 HCC in Cirrhosis XI – Diffuse Within the Entire Liver with Portal Vein Thrombosis
- •53 HCC in Cirrhosis XII – With Intrahepatic Bile Duct Dilatation
- •54 Focal Nodular Hyperplasia I – Typical with Large Central Scar and Septa
- •55 Focal Nodular Hyperplasia II – Typical with Pathologic Correlation
- •57 Focal Nodular Hyperplasia IV – Multiple FNH Syndrome
- •58 Focal Nodular Hyperplasia V – Fatty FNH with Concurrent Fatty Adenoma
- •59 Focal Nodular Hyperplasia VI – Atypical with T2 Dark Central Scar
- •60 Hepatic Angiomyolipoma – MR-CT Comparison
- •61 Hepatic Lipoma – MR-CT-US Comparison
- •62 Hepatocellular Adenoma I – Typical with Pathologic Correlation
- •63 Hepatocellular Adenoma II – Large Exophytic with Pathologic Correlation
- •64 Hepatocellular Adenoma III – Typical Fat-Containing
- •65 Hepatocellular Adenoma IV – With Large Hemorrhage
- •77 Intrahepatic Cholangiocarcinoma – With Pathologic Correlation
- •78 Telangiectatic Hepatocellular Lesion
- •79 Focal Fatty Infiltration Mimicking Metastases
- •80 Focal Fatty Sparing Mimicking Liver Lesions
- •81 Hemosiderosis – Iron Deposition, Acquired Type
- •82 Hemochromatosis – Severe Type
- •83 Hemochromatosis with Solitary HCC
- •84 Hemochromatosis with Multiple HCC
- •85 Thalassemia with Iron Deposition
- •86 Arterioportal Shunt I – Early Enhancing Lesion in a Cirrhotic Liver
- •89 Budd-Chiari Syndrome II – Gradual Deformation of the Liver
- •90 Budd-Chiari Syndrome III – Nodules Mimicking Malignancy
- •92 Caroli’s Disease I – Intrahepatic with Segmental Changes
- •93 Caroli’s Disease II – Involvement of the Liver and Kidneys
- •95 Choledocholithiasis (Bile Duct Stones)
- •96 Gallbladder Carcinoma I – Versus Gallbladder Wall Edema
- •97 Gallbladder Carcinoma II – Hepatoid Type of Adenocarcinoma
- •98 Hilar Cholangiocarcinoma I – Typical
- •99 Hilar Cholangiocarcinoma II – Intrahepatic Mass
- •100 Hilar Cholangiocarcinoma III – Partially Extrahepatic Tumor
- •101 Hilar Cholangiocarcinoma IV – Metal Stent with Interval Growth
- •102 Hilar Cholangiocarcinoma V – Biliary Dilatation Mimicking Klatskin Tumor at CT
- •103 Primary Sclerosing Cholangitis I – Cholangitis and Segmental Atrophy
- •104 Primary Sclerosing Cholangitis II – With Intrahepatic Cholestasis
- •105 Primary Sclerosing Cholangitis III – With Intrahepatic Stones
- •106 Primary Sclerosing Cholangitis IV – With Biliary Cirrhosis
- •107 Primary Sclerosing Cholangitis V – With Intrahepatic Cholangiocarcinoma
- •108 Primary Sclerosing Cholangitis VI – With Hilar Cholangiocarcinoma
- •109 T2 Bright Liver Lesions
- •110 T1 Bright Liver Lesions
- •111 T2 Bright Central Scar
- •112 Lesions in Fatty Liver
- •113 Appendix I: MR Imaging Technique and Protocol
- •114 Appendix II: Liver Segmental and Vascular Anatomy
- •Subject Index

72 Part IIB – Metastases: Non-Colorectal
34 Renal Cell Carcinoma Liver Metastasis
Renal cell carcinoma (RCC) is the 7th leading malignant condition among men and the 12th among women, accounting for 2.6 % of all cancers. The aim of preoperative imaging in RCC is to adequately assess tumor size, localization and organ confinement, to identify lymph node and/or visceral metastases, and to reliably predict the presence and extent of any thrombus of the vena cava. In 25 % of patients, advanced disease, including locally invasive or metastatic re- nal-cell carcinoma, is found at presentation. Moreover, a third of the patients who undergo resection of localized disease will have a recurrence. Median survival for patients with metastatic disease is about 13 months. Thus, there is a great need for more effective surgical and medical therapies. Nephrectomy may be warranted, even in the presence of metastatic disease. The detection of visceral metastases appears to be crucial since it has been shown that even patients with metastatic disease might benefit from radical nephrectomy followed by systemic immunotherapy. MR imaging provides more comprehensive locoregional evaluation of the primary lesion(s) including the distinction from concurrent (complicated) renal cysts, vascular invasion, and liver metastases.
Literature
1.Semelka RC, Shoenut JP, Magro CM, et al. (1993) Renal cancer staging: comparison of contrast-enhanced CT and gadolinium-enhanced fatsuppressed spin-echo and gradient-echo MR imaging. JMRI 3:597 – 602
2.Heidenreich A, Ravery V (2004) European Society of Oncological Urology: preoperative imaging in renal cell cancer. World J Urol 22:307 – 15
3.Mickisch GH, Garin A, van Poppel H, et al. (2001) Radical nephrectomy plus interferon-alfa-based immunotherapy compared with interferon alfa alone in metastatic renal-cell carcinoma: a randomized trial. Lancet 358:966 – 70
4.Figlin RA (1999) Renal cell carcinoma: management of advanced disease. J Urol 161:381 – 6
MR Imaging Findings
At MR imaging, renal cell carcinoma liver metastases appear low signal intensity on T1-weighted images and moderately high signal intensity on T2-weighted images with fat suppression. After administration of gadolinium, renal cell carcinoma liver metastases may show variable enhancement patterns including an intense homogeneous to heterogeneous enhancement in the arterial phase. In the portal and delayed phase the metastases often show washout and may become more heterogeneous (Figs. 34.1, 34.2).
Differential Diagnosis
Other hypervascular liver lesions including primary tumors as well as secondary tumors from other sources such as pancreas may have very similar appearance and need clinical correlation or US-guided biopsy for confirmation of proper diagnosis (Fig. 34.3).
Management
Surgical excision of a solitary metastasis in patients with advanced RCC is recommended in many cases, but this approach has not yet been proved to be effective in prolonging survival.
34 Renal Cell Carcinoma Liver Metastasis 73
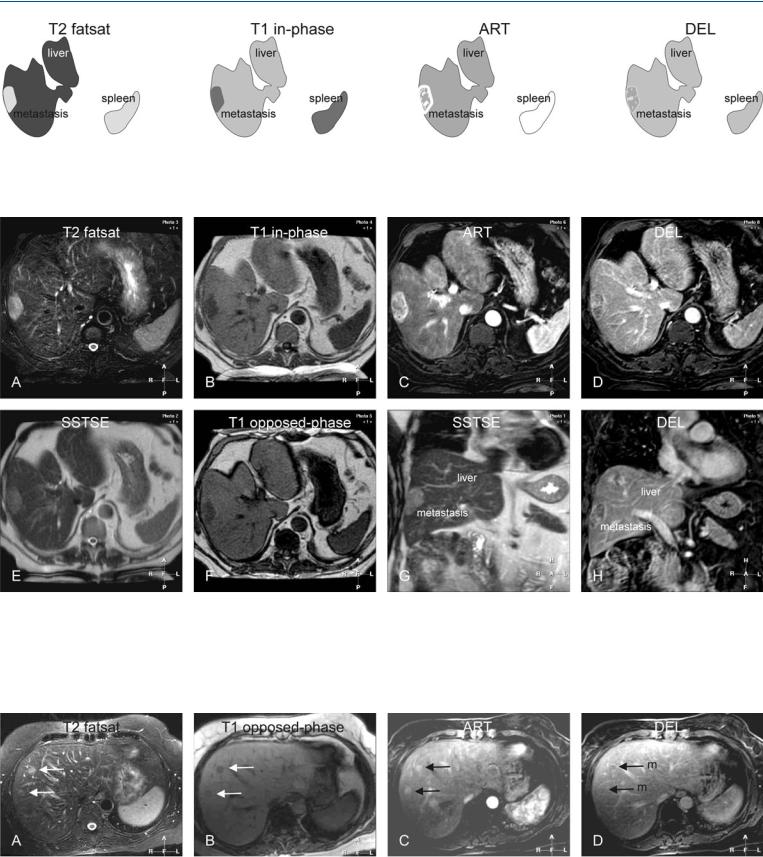
Fig. 34.1. Metastasis, renal cell carcinoma metastasis, drawings. T2 fatsat: Metastasis is hyperintense to the liver; T1 in-phase: metastasis is hypointense to the liver; ART: metastasis shows intense heterogeneous enhancement;
Fig. 34.2. Metastasis, renal cell carcinoma metastasis, MRI findings. A Axial TSE image (T2 fatsat): Metastasis is hyperintense to the liver. B Axial in-phase image (T1 in-phase): Metastasis is hypointense to the liver. C Axial arterial phase image (ART): Metastasis shows heterogeneous enhancement. D Axial delayed phase image (DEL): Metastasis shows some washout with persistent heterogeneous enhancement. E Axial SSTSE image (SSTSE): Metastasis is
DEL: metastasis shows some washout with persistent heterogeneous enhancement
slightly hyperintense. F Axial opposed-phase image (T1 opposed-phase) shows slight signal drop in the liver indicating subtle steatosis. Note that metastases are surrounded by persistent high perifocal signal due to compressed liver. G Coronal SSTSE image (SSTSE) shows the metastasis as a relatively bright lesion. H Coronal delayed image (DEL) shows the metastasis with persistent heterogeneous enhancement
Fig. 34.3. Metastases, pancreas carcinoma metastases (another patient), MRI findings. A Axial TSE image (T2 fatsat) shows two metastases that are slightly hyperintense to the liver (arrows). B Axial opposed-phase image (T1 op- posed-phase): metastases are hypointense to the liver (arrows). C Axial arte-
rial phase image (ART): metastases show faint, homogenous enhancement (arrows). D Axial delayed phase image (DEL) shows washout within lesions
(m).

Part II/IIC
Solid Liver Lesions |
II |
Primary Solid Liver Lesions in Cirrhotic Liver |
IIB |
