
- •Dedication
- •Editors and Contributors
- •Foreword
- •Preface
- •Contents
- •PREPARING FOR THE SURGERY CLERKSHIP
- •SURGICAL NOTES
- •COMMON ABBREVIATIONS YOU SHOULD KNOW
- •RETRACTORS (YOU WILL GET TO KNOW THEM WELL!)
- •SUTURE MATERIALS
- •WOUND CLOSURE
- •KNOTS AND EARS
- •INSTRUMENT TIE
- •TWO-HAND TIE
- •COMMON PROCEDURES
- •NASOGASTRIC TUBE (NGT) PROCEDURES
- •CHEST TUBES
- •NASOGASTRIC TUBES (NGT)
- •FOLEY CATHETER
- •CENTRAL LINES
- •MISCELLANEOUS
- •THIRD SPACING
- •COMMON IV REPLACEMENT FLUIDS (ALL VALUES ARE PER LITER)
- •CALCULATION OF MAINTENANCE FLUIDS
- •ELECTROLYTE IMBALANCES
- •ANTIBIOTICS
- •STEROIDS
- •HEPARIN
- •WARFARIN (COUMADIN®)
- •MISCELLANEOUS AGENTS
- •NARCOTICS
- •MISCELLANEOUS
- •ATELECTASIS
- •POSTOPERATIVE RESPIRATORY FAILURE
- •PULMONARY EMBOLISM
- •ASPIRATION PNEUMONIA
- •GASTROINTESTINAL COMPLICATIONS
- •ENDOCRINE COMPLICATIONS
- •CARDIOVASCULAR COMPLICATIONS
- •MISCELLANEOUS
- •HYPOVOLEMIC SHOCK
- •SEPTIC SHOCK
- •CARDIOGENIC SHOCK
- •NEUROGENIC SHOCK
- •MISCELLANEOUS
- •URINARY TRACT INFECTION (UTI)
- •CENTRAL LINE INFECTIONS
- •WOUND INFECTION (SURGICAL SITE INFECTION)
- •NECROTIZING FASCIITIS
- •CLOSTRIDIAL MYOSITIS
- •SUPPURATIVE HIDRADENITIS
- •PSEUDOMEMBRANOUS COLITIS
- •PROPHYLACTIC ANTIBIOTICS
- •PAROTITIS
- •MISCELLANEOUS
- •CHEST
- •ABDOMEN
- •MALIGNANT HYPERTHERMIA
- •MISCELLANEOUS
- •OVERVIEW
- •CHOLECYSTOKININ (CCK)
- •SECRETIN
- •GASTRIN
- •SOMATOSTATIN
- •MISCELLANEOUS
- •GROIN HERNIAS
- •HERNIA REVIEW QUESTIONS
- •ESOPHAGEAL HIATAL HERNIAS
- •PRIMARY SURVEY
- •SECONDARY SURVEY
- •TRAUMA STUDIES
- •PENETRATING NECK INJURIES
- •MISCELLANEOUS TRAUMA FACTS
- •PEPTIC ULCER DISEASE (PUD)
- •DUODENAL ULCERS
- •GASTRIC ULCERS
- •PERFORATED PEPTIC ULCER
- •TYPES OF SURGERIES
- •STRESS GASTRITIS
- •MALLORY-WEISS SYNDROME
- •ESOPHAGEAL VARICEAL BLEEDING
- •BOERHAAVE’S SYNDROME
- •ANATOMY
- •GASTRIC PHYSIOLOGY
- •GASTROESOPHAGEAL REFLUX DISEASE (GERD)
- •GASTRIC CANCER
- •GIST
- •MALTOMA
- •GASTRIC VOLVULUS
- •SMALL BOWEL
- •APPENDICITIS
- •CLASSIC INTRAOPERATIVE QUESTIONS
- •APPENDICEAL TUMORS
- •SPECIFIC TYPES OF FISTULAS
- •ANATOMY
- •COLORECTAL CARCINOMA
- •COLONIC AND RECTAL POLYPS
- •POLYPOSIS SYNDROMES
- •DIVERTICULAR DISEASE OF THE COLON
- •ANATOMY
- •ANAL CANCER
- •ANATOMY
- •TUMORS OF THE LIVER
- •ABSCESSES OF THE LIVER
- •HEMOBILIA
- •ANATOMY
- •PHYSIOLOGY
- •PATHOPHYSIOLOGY
- •DIAGNOSTIC STUDIES
- •BILIARY SURGERY
- •OBSTRUCTIVE JAUNDICE
- •CHOLELITHIASIS
- •ACUTE CHOLECYSTITIS
- •ACUTE ACALCULOUS CHOLECYSTITIS
- •CHOLANGITIS
- •SCLEROSING CHOLANGITIS
- •GALLSTONE ILEUS
- •CARCINOMA OF THE GALLBLADDER
- •CHOLANGIOCARCINOMA
- •MISCELLANEOUS CONDITIONS
- •PANCREATITIS
- •PANCREATIC ABSCESS
- •PANCREATIC NECROSIS
- •PANCREATIC PSEUDOCYST
- •PANCREATIC CARCINOMA
- •MISCELLANEOUS
- •ANATOMY OF THE BREAST AND AXILLA
- •BREAST CANCER
- •DCIS
- •LCIS
- •MISCELLANEOUS
- •MALE BREAST CANCER
- •BENIGN BREAST DISEASE
- •CYSTOSARCOMA PHYLLODES
- •FIBROADENOMA
- •FIBROCYSTIC DISEASE
- •MASTITIS
- •BREAST ABSCESS
- •MALE GYNECOMASTIA
- •ADRENAL GLAND
- •ADDISON’S DISEASE
- •INSULINOMA
- •GLUCAGONOMA
- •SOMATOSTATINOMA
- •ZOLLINGER-ELLISON SYNDROME (ZES)
- •MULTIPLE ENDOCRINE NEOPLASIA
- •THYROID DISEASE
- •ANATOMY
- •PHYSIOLOGY
- •HYPERPARATHYROIDISM (HPTH)
- •PARATHYROID CARCINOMA
- •SOFT TISSUE SARCOMAS
- •LYMPHOMA
- •SQUAMOUS CELL CARCINOMA
- •BASAL CELL CARCINOMA
- •MISCELLANEOUS SKIN LESIONS
- •STAGING
- •INTENSIVE CARE UNIT (ICU) BASICS
- •INTENSIVE CARE UNIT FORMULAS AND TERMS YOU SHOULD KNOW
- •SICU DRUGS
- •INTENSIVE CARE PHYSIOLOGY
- •HEMODYNAMIC MONITORING
- •MECHANICAL VENTILATION
- •PERIPHERAL VASCULAR DISEASE
- •LOWER EXTREMITY AMPUTATIONS
- •ACUTE ARTERIAL OCCLUSION
- •ABDOMINAL AORTIC ANEURYSMS
- •MESENTERIC ISCHEMIA
- •MEDIAN ARCUATE LIGAMENT SYNDROME
- •CAROTID VASCULAR DISEASE
- •CLASSIC CEA INTRAOP QUESTIONS
- •SUBCLAVIAN STEAL SYNDROME
- •RENAL ARTERY STENOSIS
- •SPLENIC ARTERY ANEURYSM
- •POPLITEAL ARTERY ANEURYSM
- •MISCELLANEOUS
- •PEDIATRIC IV FLUIDS AND NUTRITION
- •PEDIATRIC BLOOD VOLUMES
- •FETAL CIRCULATION
- •ECMO
- •NECK
- •ASPIRATED FOREIGN BODY (FB)
- •CHEST
- •PULMONARY SEQUESTRATION
- •ABDOMEN
- •INGUINAL HERNIA
- •UMBILICAL HERNIA
- •GERD
- •CONGENITAL PYLORIC STENOSIS
- •DUODENAL ATRESIA
- •MECONIUM ILEUS
- •MECONIUM PERITONITIS
- •MECONIUM PLUG SYNDROME
- •ANORECTAL MALFORMATIONS
- •HIRSCHSPRUNG’S DISEASE
- •MALROTATION AND MIDGUT VOLVULUS
- •OMPHALOCELE
- •GASTROSCHISIS
- •POWER REVIEW OF OMPHALOCELE AND GASTROSCHISIS
- •APPENDICITIS
- •INTUSSUSCEPTION
- •MECKEL’S DIVERTICULUM
- •NECROTIZING ENTEROCOLITIS
- •BILIARY TRACT
- •TUMORS
- •PEDIATRIC TRAUMA
- •OTHER PEDIATRIC SURGERY QUESTIONS
- •POWER REVIEW
- •WOUND HEALING
- •SKIN GRAFTS
- •FLAPS
- •SENSORY SUPPLY TO THE HAND
- •CARPAL TUNNEL SYNDROME
- •ANATOMY
- •MISCELLANEOUS
- •NOSE AND PARANASAL SINUSES
- •ORAL CAVITY AND PHARYNX
- •FACIAL FRACTURES
- •ENT WARD QUESTIONS
- •RAPID-FIRE REVIEW OF MOST COMMON CAUSES OF ENT INFECTIONS
- •THORACIC OUTLET SYNDROME (TOS)
- •CHEST WALL TUMORS
- •DISEASES OF THE PLEURA
- •DISEASES OF THE LUNGS
- •DISEASES OF THE MEDIASTINUM
- •DISEASES OF THE ESOPHAGUS
- •ACQUIRED HEART DISEASE
- •CONGENITAL HEART DISEASE
- •CARDIAC TUMORS
- •DISEASES OF THE GREAT VESSELS
- •MISCELLANEOUS
- •BASIC IMMUNOLOGY
- •CELLS
- •IMMUNOSUPPRESSION
- •OVERVIEW OF IMMUNOSUPPRESSION MECHANISMS
- •MATCHING OF DONOR AND RECIPIENT
- •REJECTION
- •ORGAN PRESERVATION
- •KIDNEY TRANSPLANT
- •LIVER TRANSPLANT
- •PANCREAS TRANSPLANT
- •HEART TRANSPLANT
- •INTESTINAL TRANSPLANTATION
- •LUNG TRANSPLANT
- •TRANSPLANT COMPLICATIONS
- •ORTHOPAEDIC TERMS
- •TRAUMA GENERAL PRINCIPLES
- •FRACTURES
- •ORTHOPAEDIC TRAUMA
- •DISLOCATIONS
- •THE KNEE
- •ACHILLES TENDON RUPTURE
- •ROTATOR CUFF
- •MISCELLANEOUS
- •ORTHOPAEDIC INFECTIONS
- •ORTHOPAEDIC TUMORS
- •ARTHRITIS
- •PEDIATRIC ORTHOPAEDICS
- •HEAD TRAUMA
- •SPINAL CORD TRAUMA
- •TUMORS
- •VASCULAR NEUROSURGERY
- •SPINE
- •PEDIATRIC NEUROSURGERY
- •SCROTAL ANATOMY
- •UROLOGIC DIFFERENTIAL DIAGNOSIS
- •RENAL CELL CARCINOMA (RCC)
- •BLADDER CANCER
- •PROSTATE CANCER
- •BENIGN PROSTATIC HYPERPLASIA
- •TESTICULAR CANCER
- •TESTICULAR TORSION
- •EPIDIDYMITIS
- •PRIAPISM
- •ERECTILE DYSFUNCTION
- •CALCULUS DISEASE
- •INCONTINENCE
- •URINARY TRACT INFECTION (UTI)
- •MISCELLANEOUS UROLOGY QUESTIONS
- •Rapid Fire Power Review
- •TOP 100 CLINICAL SURGICAL MICROVIGNETTES
- •Figure Credits
- •Index

152 Section I / Overview and Background Surgical Information
What is the treatment? ASA, heparin if feasible postoperatively Thrombolytic therapy is not usually postoperative option
What is the perioperative prevention?
MISCELLANEOUS
Avoid hypotension; continue aspirin therapy preoperatively in high-risk patients if feasible; preoperative carotid Doppler study in high-risk patients
POSTOPERATIVE RENAL FAILURE
What is it? |
Increase in serum creatinine and |
|
decrease in creatinine clearance; usually |
|
associated with decreased urine output |
Define the following terms: |
|
Anuria |
50 cc urine output in 24 hours |
Oliguria |
Between 50 cc and 400 cc of urine |
|
output in 24 hours |
What is the differential |
|
diagnosis? |
|
Prerenal |
Inadequate blood perfusing kidney: |
|
inadequate fluids, hypotension, cardiac |
|
pump failure (CHF) |
Renal |
Kidney parenchymal dysfunction: |
|
acute tubular necrosis, nephrotoxic |
|
contrast or drugs |
Postrenal |
Obstruction to outflow of urine from |
|
kidney: Foley catheter obstruction/stone, |
|
ureteral/urethral injury, BPH, bladder |
|
dysfunction (e.g., medications, spinal |
|
anesthesia) |
What is the workup? |
Lab tests: electrolytes, BUN, Cr, urine |
|
lytes/Cr, FENa, urinalysis, renal ultrasound |
What is FENa? |
Fractional Excretion of Na (sodium) |

What is the formula for FENa?
Define the lab results with prerenal vs renal failure:
BUN/Cr ratio
Specific gravity
Chapter 22 / Complications 153
“YOU NEED PEE” UNP
(UNa Pcr / PNa Ucr) 100
(U urine, cr creatinine, Na sodium, P plasma)
Prerenal: 20:1
Renal: 20:1
Prerenal: 1.020 (as the body tries to hold on to fluid)
Renal: 1.020 (kidney has decreased ability to concentrate urine)
FENa
Urine Na (sodium)
Urine osmolality
What are the indications for dialysis?
DIC
Prerenal: 1%
Renal: 2%
Prerenal: 20
Renal: 40
Prerenal: 450
Renal: 300 mOsm/kg
Fluid overload, refractory hyperkalemia, BUN 130, acidosis, uremic complication (encephalopathy, pericardial effusion)
What is it? |
Activation of the coagulation cascade |
|
leading to thrombosis and consumption |
|
of clotting factors and platelets and |
|
activation of fibrinolytic system |
|
(fibrinolysis), resulting in bleeding |
What are the causes? |
Tissue necrosis, septic shock, massive |
|
large-vessel coagulation, shock, allergic |
|
reactions, massive blood transfusion |
|
reaction, cardiopulmonary bypass, cancer, |
|
obstetric complications, snake bites, |
|
trauma, burn injury, prosthetic material, |
|
liver dysfunction |
154 Section I / Overview and Background Surgical Information
What are the signs/ |
Acrocyanosis or other signs of thrombosis, |
symptoms? |
then diffuse bleeding from incision sites, |
|
venipuncture sites, catheter sites, or |
|
mucous membranes |
What are the associated lab findings?
Increased fibrin-degradation products, elevated PT/PTT, decreased platelets, decreased fibrinogen (level correlates well with bleeding), presence of schistocytes (fragmented RBCs), increased D-dimer
What is the treatment? |
Removal of the cause; otherwise |
|
supportive: IVFs, O2, platelets, FFP, |
|
cryoprecipitate (fibrin), Epsilon- |
|
aminocaproic acid, as needed in |
|
predominantly thrombotic cases |
|
Use of heparin is indicated in cases that |
|
are predominantly thrombotic with |
|
antithrombin III supplementation as |
|
needed |
ABDOMINAL COMPARTMENT SYNDROME |
|
|
|
What is it? |
Increased intra-abdominal pressure |
|
usually seen after laparotomy or after |
massive IVF resuscitation (e.g., burn patients)
What are the signs/ symptoms?
How to measure intraabdominal pressure?
What is normal intraabdominal pressure?
What intra-abdominal pressure indicates need for treatment?
What is the treatment?
Tight distended abdomen, decreased urine output, increased airway pressure, increased intra-abdominal pressure
Read intrabladder pressure (Foley catheter hooked up to manometry after instillation of 50–100 cc of water)
15 mm Hg
25 mm Hg, especially if signs of compromise
Release the pressure by placing drain and/or decompressive laparotomy (leaving fascia open)

What is a “Bogata Bag”?
Chapter 22 / Complications 155
Sheet of plastic (empty urology irrigation bag or IV bag) used to temporarily close the abdomen to allow for more intraabdominal volume
URINARY RETENTION
What is it? |
Enlarged urinary bladder resulting from |
|
medications or spinal anesthesia |
How is it diagnosed? |
Physical exam (palpable bladder), bladder |
|
residual volume upon placement of a |
|
Foley catheter |
What is the treatment? |
Foley catheter |
With massive bladder |
Most would clamp after 1 L and then |
distention, how much urine |
drain the rest over time to avoid a |
can be drained immediately? |
vasovagal reaction |
What is the classic sign of |
Confusion |
urinary retention in an |
|
elderly patient? |
|
WOUND INFECTION |
|
|
|
What are the signs/ |
Erythema, swelling, pain, heat (rubor, |
symptoms? |
tumor, dolor, calor) |
What is the treatment? |
Open wound, leave open with wet to dry |
|
dressing changes, antibiotics if cellulitis |
|
present |
What is fascial dehiscence? |
Acute separation of fascia that has been |
|
sutured closed |
What is the treatment? |
Bring back to the O.R. emergently for |
|
reclosure of the fascia |
WOUND HEMATOMA |
|
|
|
What is it? |
Collection of blood (blood clot) in |
|
operative wound |
What is the treatment? |
Acute: Remove with hemostasis |
|
Subacute: Observe (heat helps resorption) |

156 Section I / Overview and Background Surgical Information
WOUND SEROMA
What is it? |
Postoperative collection of lymph and |
|
serum in the operative wound |
What is the treatment? |
Needle aspiration, repeat if necessary |
|
(prevent with closed drain) |
PSEUDOMEMBRANOUS COLITIS |
|
|
|
What are the signs/ |
Diarrhea, fever, hypotension/tachycardia |
symptoms? |
|
What is the incidence of |
10% |
bloody diarrhea? |
|
What classic antibiotic |
Clindamycin (but almost all antibiotics |
causes C. difficile? |
can cause it) |
How is it diagnosed? |
C. diff toxin in stool, fecal WBC, flex sig |
|
(see a mucous pseudomembrane in |
|
lumen of colon hence the name) |
What is the treatment? |
1. Flagyl (PO or IV) |
|
2. PO vancomycin if refractory to Flagyl |
What is the indication for |
Toxic megacolon |
emergent colectomy? |
|
C h a p t e r 23
Common
Causes of Ward
Emergencies
What can cause |
Hypovolemia (iatrogenic, hemorrhage), |
hypotension? |
sepsis, MI, cardiac dysrhythmia, hypoxia, |
|
false reading (e.g., wrong cuff/arterial |
|
line twist or clot), pneumothorax, PE, |
|
cardiac tamponade, medications (e.g., |
|
morphine) |
Chapter 23 / Common Causes of Ward Emergencies 157
How do you act? |
ABCs, examine, recheck BP, IV access, |
|
IV bolus, labs (e.g., HCT), EKG, pulse |
|
ox/vital signs monitoring, CXR, supple- |
|
mental oxygen, check medications/history, |
|
give IV antibiotics “stat” if sepsis likely, |
|
compress all bleeding sites |
What are the common |
Pain (from catecholamine release), anxiety, |
causes of postoperative |
hypercapnia, hypoxia (which may also |
hypertension? |
cause hypotension), preexisting condition, |
|
bladder distention |
What can cause hypoxia/ |
Atelectasis, pneumonia, mucous plug, |
shortness of breath? |
pneumothorax, PE, MI/dysrhythmia, |
|
venous blood in ABG syringe, SAT% |
|
machine malfunction/probe malposition, |
|
iatrogenic (wrong ventilator settings), |
|
severe anemia/hypovolemia, low |
|
cardiac output, CHF, ARDS, fluid |
|
overload |
How do you act? |
ABCs, physical exam, vital signs/pulse |
|
oximetry monitoring, supplemental |
|
oxygen, IV access, ABG, EKG, CXR |
What can cause mental |
Hypoxia until ruled out, hypotension |
status change? |
(e.g., cardiogenic shock), hypovolemia, |
|
iatrogenic (narcotics/benzodiazepines), |
|
drug reaction, alcohol withdrawal, drug |
|
withdrawal, seizure, ICU psychosis, |
|
CVA, sepsis, metabolic derangements, |
|
intracranial bleeding, urinary retention |
|
in the elderly |
What are the signs of |
Confusion, tachycardia/autonomic |
alcohol withdrawal? |
instability, seizure, hallucinations |
What are the causes of |
Hypovolemia/third-spacing, pain, |
tachycardia? |
alcohol withdrawal, anxiety/agitation, |
|
urinary retention, cardiac dysrhythmia |
|
(e.g., sinoventricular tachycardia, atrial |
|
fibrillation with rapid rate), MI, PE, |
|
-blocker withdrawal, anastomotic |
|
leak |

158 Section I / Overview and Background Surgical Information
What are the causes of decreased urine output?
Hypovolemia, urinary retention, Foley catheter malfunction, cardiac failure, MI, acute tubular necrosis (ATN), ureteral/urethral injury, abdominal compartment syndrome, sepsis
How do you act initially in a case of decreased urine output?
Examine, vital signs, check or place Foley catheter, irrigate Foley catheter, IV fluid bolus
C h a p t e r 24
What is the most common cause of fever in the first 48 hours postop?
What is absorption atelectasis?
What is incentive spirometry?
Surgical
Respiratory Care
Atelectasis
Elevated inhaled oxygen replaces the nitrogen in the alveoli resulting in collapse of the air sac (atelectasis); nitrogen keeps alveoli open by “stenting” them
Patient can document tidal volume and will have an “incentive” to increase it
h r f
'
0 4

What is oxygen-induced hypoventilation?
Why give supplemental oxygen to a patient with a pneumothorax?
What is a nonrebreather mask?
Chapter 24 / Surgical Respiratory Care 159
Some patients with COPD have low oxygen as the main stimulus for the respiratory drive; if given supplemental oxygen, they will have a decreased respiratory drive and hypoventilation
Pneumothorax is almost completely nitrogen—thus increasing the oxygen in the alveoli increases the nitrogen gradient and results in faster absorption of the pneumothorax!
100% oxygen with a reservoir bag
Exhalation 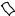 valve
valve  opens
opens 
Valve  closes
closes
Reservoir bag expands fully
Why do nonrebreather masks have a “reservoir” bag?
What is the maximum oxygen FiO2 delivered by a nonrebreather mask?
How do you figure out the PaO2 from an O2 sat?
Inhalation flow will exceed the delivery rate of the tubing and the bag allows for extra oxygen stores
80% to 90%
PaO2 of 40, 50, 60 roughly equals 70, 80, 90 in sats

160 Section I / Overview and Background Surgical Information
What is an oxygen nasal cannula?
Oxygen delivered via tubing with prongs into nares
How much do you increase |
3% |
the FiO2 by each liter added |
|
to the nasal cannula? |
|
What is the max effective |
6 liters |
flow for a nasal cannula? |
|
C h a p t e r 25 |
Surgical Nutrition |
What is the motto of surgical |
“If the gut works, use it” |
nutrition? |
|
What are the normal daily |
|
dietary requirements for |
|
adults of the following: |
|
Protein |
1 g/kg/day |
Calories |
30 kcal/kg/day |
|
Chapter 25 / Surgical Nutrition 161 |
By how much is basal |
|
energy expenditure (BEE) |
|
increased or decreased in |
|
the following cases: |
Increased 1.7 |
Severe head injury |
|
Severe burns |
Increased 2–3 |
What are the calorie contents |
|
of the following substances: |
|
Fat |
9 kcal/g |
Protein |
4 kcal/g |
Carbohydrate |
4 kcal/g |
What is the formula for |
Nitrogen 6.25 protein |
converting nitrogen |
|
requirement/loss to protein |
|
requirement/loss? |
|
What is RQ? |
Respiratory Quotient: ratio of CO2 |
|
produced to O2 consumed |
What is the normal RQ? |
0.8 |
What can be done to |
More fat, less carbohydrates |
decrease the RQ? |
|
What dietary change can be |
Decrease carbohydrate calories and |
made to decrease CO2 pro- |
increase calories from fat |
duction in a patient in whom |
|
CO2 retention is a concern? |
|
What lab tests are used to |
Blood levels of: |
monitor nutritional status? |
Prealbumin (t1/2 2–3 days)—acute |
|
change determination |
|
Transferrin (t1/2 8–9 days) |
|
Albumin (t1/2 14–20 days)—more |
|
chronic determination |
|
Total lymphocyte count |
|
Anergy |
|
Retinol-binding protein (t1/2 12 |
|
hours) |
Where is iron absorbed? |
Duodenum (some in proximal jejunum) |
162 Section I / Overview and Background Surgical Information
Where is vitamin B12 absorbed?
What are the surgical causes of vitamin B12 deficiency?
Where are bile salts absorbed?
Where are fat-soluble vitamins absorbed?
Which vitamins are fat soluble?
What are the signs of the following disorders:
Vitamin A deficiency
Vitamin B12/folate deficiency
Vitamin C deficiency
Vitamin K deficiency
Terminal ileum
Gastrectomy, excision of terminal ileum, blind loop syndrome
Terminal ileum
Terminal ileum
K, A, D, E (“KADE”)
Poor wound healing
Megaloblastic anemia
Poor wound healing, bleeding gums
T in the vitamin K–dependent clotting factors (II, VII, IX, and X); bleeding; elevated PT
Chromium deficiency
Zinc deficiency
Fatty acid deficiency
What vitamin increases the PO absorption of iron?
What vitamin lessens the deleterious effects of steroids on wound healing?
What are the common indications for total parenteral nutrition (TPN)?
Diabetic state
Poor wound healing, alopecia, dermatitis, taste disorder
Dry, flaky skin; alopecia
PO vitamin C (ascorbic acid)
Vitamin A
NPO 7 days
Enterocutaneous fistulas
Short bowel syndrome
Prolonged ileus
What is TPN?
What is in TPN?
How much of each in TPN: Lipids
Protein
Carbohydrates
What are the possible complications of TPN?
Chapter 25 / Surgical Nutrition 163
Total Parenteral Nutrition IV nutrition
Protein Carbohydrates Lipids
(H2O, electrolytes, minerals/vitamins,insulin, H2 blocker)
20% to 30% of calories (lipid from soybeans, etc.)
1.7 g/kg/day (10%–20% of calories) as amino acids
50% to 60% of calories as dextrose
Line infection, fatty infiltration of the liver, electrolyte/glucose problems, pneumothorax during placement of central line, loss of gut barrier, acalculus cholecystitis, refeeding syndrome, hyperosmolality
What are the advantages of enteral feeding?
Keeps gut barrier healthy, thought to lessen translocation of bacteria, not associated with complications of line placement, associated with fewer electrolyte/glucose problems
What is the major nutrient of the gut (small bowel)?
What is “refeeding syndrome”?
Glutamine
Decreased serum potassium, magnesium, and phosphate after refeeding (via TPN or enterally) a starving patient
What are the vitamin K–dependent clotting factors?
What is an elemental tube feed?
Where is calcium absorbed?
2, 7, 9, 10 (Think: 2 7 9, and then 10)
Very low residue tube feed in which almost all the tube feed is absorbed
Duodenum (actively)
Jejunum (passively)

164 Section I / Overview and Background Surgical Information
What is the major nutrient |
Butyrate (and other short-chain fatty |
of the colon? |
acids) |
What must bind B12 for |
Intrinsic factor from the gastric parietal |
absorption? |
cells |
What sedative medication |
Propofol delivers 1 kcal/cc in the form of |
has caloric value? |
lipid! |
Why may all the insulin |
Insulin will bind to the IV tubing |
placed in a TPN bag not get |
|
to the patient? |
|
What is the best way to deter- |
Metabolic chart |
mine the caloric requirements |
|
of a patient on the ventilator? |
|
How can serum bicarbonate be increased in patients on TPN?
What are “trophic” tube feeds?
When should PO feedings be started after a laparotomy?
What is the best parameter to check adequacy of nutritional status?
Increase acetate (which is metabolized into bicarbonate)
Very low rate of tube feeds (usually 10–25 cc/hr), which are thought to keep mucosa alive and healthy
Classically after flatus or stool PR (usually postoperative days 3–5)
Prealbumin
C h a p t e r 26 |
Shock |
What is the definition of |
Inadequate tissue perfusion |
shock? |
|
What are the different |
Hypovolemic |
types (5)? |
Septic |
|
Cardiogenic |
|
Neurogenic |
|
Anaphylactic |
