
- •Preface
- •Acknowledgements
- •Contents
- •The Team
- •The Instruments
- •Patient Positioning
- •Setup for Upper Abdominal Surgery
- •Setup for Lower Abdominal Surgery
- •The Working Environment
- •Appraisal of Surgical Instruments
- •Trocars
- •Other Instrumental Requirements
- •Troubleshooting Loss of Pneumoperitoneum
- •Principles of Hemostasis
- •Control of Bleeding of Unnamed Vessels
- •Control of Bleeding of a Main Named Vessel
- •Selected Further Reading
- •2 Cholecystectomy
- •Impacted Stone (Hydrops, Empyema, Early Mirizzi)
- •Adhesions Due to Previous Upper Midline Laparotomy
- •Selected Further Reading
- •Selected Further Reading
- •The Need for Specialized Equipment
- •Access to the Liver
- •Maneuvers Common to All Laparoscopic Liver Surgery
- •Resection of Liver Tumors
- •Limited Resection of Minor Lesions
- •Left Lateral Segmentectomy
- •Right Hepatectomy
- •Patient Selection
- •Principles of Surgical Therapy in the Management of Gastroesophageal Reflux Disease
- •Patient Positioning
- •Technique
- •Postoperative Course
- •Management of Complications
- •Paraesophageal Hernia
- •Esophageal Myotomy for Achalasia
- •Vagotomies
- •Bilateral Truncal Vagotomy
- •Highly Selective Vagotomy
- •Lesser Curvature Seromyotomy and Posterior Truncal Vagotomy
- •Selected Further Reading
- •Pyloroplasty
- •Vagotomy with Antrectomy or any Distal Gastrectomy
- •Port Placement
- •Technique
- •Locating the Perforation
- •Abdominal Washout
- •Closure of the Perforation with an Omental Patch
- •Postoperative Course
- •Selected Further Reading
- •7 Appendectomy
- •OR Setup and Port Placement
- •Technique
- •Gangrenous or Perforated Appendicitis
- •Laparoscopic Assisted Appendectomy
- •Left Hemicolectomy
- •Reversing the Hartmann Procedure
- •Selected Further Reading
- •Selected Further Reading
- •Transabdominal Preperitoneal Repair (TAPP)
- •Patient and Port Positioning
- •Dissection of the Preperitoneal Space
- •Dissection of the Cord Structures and the Vas Deferens
- •Placement of the Mesh and Fixation
- •Closure of the Peritoneum
- •Indications
- •Technique
- •Positioning
- •Pneumoperitoneum
- •Port Placement
- •Adhesiolysis
- •Measurement of the Hernia Defect
- •Placement of Mesh
- •Difficult Ventral or Incisional Hernias
- •Pain Following Laparoscopic Ventral or Incisional Hernia Repair
- •Preoperative Requirements and Workup
- •Patient Positioning
- •Port Placement
- •Surgical Anatomy
- •Surgical Principles
- •Technique
- •Division of the Short Gastric Vessels and Exposure of the Tail of the Pancreas
- •Division of the Hilar Vessels and Phrenic Attachments
- •Extraction of the Spleen in a Bag
- •Final Steps of the Procedure
- •Control of an Unnamed Vessel
- •Control of a Major Vessel
- •Splenic Injury
- •Maneuver of Last Resort During Bleeding of the Hilar Vessels
- •Distal Splenopancreatectomy
- •Selected Further Reading
- •13 Adrenalectomy
- •Principles
- •Patient Positioning
- •Technique
- •Immediate Postoperative Complications
- •Late Postoperative Complications
- •Laparoscopic Adjustable Band
- •Technique
- •Complications
- •Laparoscopic Sleeve Gastrectomy
- •Selected Further Reading
- •Laparoscopic Cholecystectomy
- •Laparoscopic Appendectomy
- •Laparoscopic Inguinal Hernia Repair
- •Selected Further Reading
- •Monitors
- •OR Table
- •Trocar Placement and Triangulation
- •Equipment
- •Needle Holders
- •Graspers
- •Suture Material
- •Intracorporeal Knot-Tying
- •Interrupted Stitch
- •Running Stitch
- •Pirouette
- •Extracorporeal Knot-Tying
- •Roeder’s Knot
- •Endoloop
- •Troubleshooting
- •Lost Needle
- •Short Suture
- •Subject Index
186 |
Chapter 12 Splenectomy (Total and Partial) and Splenopancreatectomy |
Port Placement
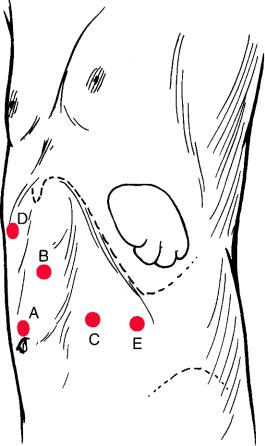
Four to five 12 mm ports are needed for this operation (Fig. 12.5). Following insufflation using a Veress needle, the first trocar is inserted in the left upper quadrant approximately five fingerbreadths below the costal margin, moving the camera closer to the spleen. This will permit full exploration of the abdominal cavity to check for the presence of accessory spleens and other intra-abdominal lesions that might require laparoscopic management.
One port is inserted on each side of the umbilical port in a triangulated manner, for the right and left hands of the surgeon. Another trocar is inserted laterally under the left costal margin for the first assistant. An optional subxiphoid trocar can be inserted for an irrigation/suction device or for a fan retractor used by the camera assistant if needed.
Fig. 12.5 Port positions for laparoscopic splenectomy: A umbilical telescope; B surgeon’s left
hand; C surgeon’s right hand; D subxiphoid port for irrigation/suction or an assistant’s grasper;
E first assistant’s grasper

Classic Laparoscopic Splenectomy |
187 |
Surgical Anatomy
Vascularization of the spleen may be of the distributed type (Fig. 12.6a) or the nonbranching variant (Fig. 12.6b). Knowledge of the patient’s vascular anatomy will help decide on the most appropriate dissection technique. The terminal branches of the splenic artery are depicted in Fig. 12.7. Knowledge of the anatomy of the spleen is critical, and two special features are of interest. First, as a rule, notched spleens and those with prominences have more entering arteries than those with smooth borders (usually distributed type). Second, the tail of the pancreas lies close to the hilum of the spleen and is in direct contact with the spleen in about 30% of cases, and within 1 cm of the spleen in 40%. Caution is therefore recommended before firing a linear cutter across the hilar vessels.
a
b
Fig. 12.6 Vascularization of the spleen: (a) distributed type with multiple splenic notches, and (b) magistral type with few splenic notches
