
- •Preface
- •Acknowledgements
- •Contents
- •The Team
- •The Instruments
- •Patient Positioning
- •Setup for Upper Abdominal Surgery
- •Setup for Lower Abdominal Surgery
- •The Working Environment
- •Appraisal of Surgical Instruments
- •Trocars
- •Other Instrumental Requirements
- •Troubleshooting Loss of Pneumoperitoneum
- •Principles of Hemostasis
- •Control of Bleeding of Unnamed Vessels
- •Control of Bleeding of a Main Named Vessel
- •Selected Further Reading
- •2 Cholecystectomy
- •Impacted Stone (Hydrops, Empyema, Early Mirizzi)
- •Adhesions Due to Previous Upper Midline Laparotomy
- •Selected Further Reading
- •Selected Further Reading
- •The Need for Specialized Equipment
- •Access to the Liver
- •Maneuvers Common to All Laparoscopic Liver Surgery
- •Resection of Liver Tumors
- •Limited Resection of Minor Lesions
- •Left Lateral Segmentectomy
- •Right Hepatectomy
- •Patient Selection
- •Principles of Surgical Therapy in the Management of Gastroesophageal Reflux Disease
- •Patient Positioning
- •Technique
- •Postoperative Course
- •Management of Complications
- •Paraesophageal Hernia
- •Esophageal Myotomy for Achalasia
- •Vagotomies
- •Bilateral Truncal Vagotomy
- •Highly Selective Vagotomy
- •Lesser Curvature Seromyotomy and Posterior Truncal Vagotomy
- •Selected Further Reading
- •Pyloroplasty
- •Vagotomy with Antrectomy or any Distal Gastrectomy
- •Port Placement
- •Technique
- •Locating the Perforation
- •Abdominal Washout
- •Closure of the Perforation with an Omental Patch
- •Postoperative Course
- •Selected Further Reading
- •7 Appendectomy
- •OR Setup and Port Placement
- •Technique
- •Gangrenous or Perforated Appendicitis
- •Laparoscopic Assisted Appendectomy
- •Left Hemicolectomy
- •Reversing the Hartmann Procedure
- •Selected Further Reading
- •Selected Further Reading
- •Transabdominal Preperitoneal Repair (TAPP)
- •Patient and Port Positioning
- •Dissection of the Preperitoneal Space
- •Dissection of the Cord Structures and the Vas Deferens
- •Placement of the Mesh and Fixation
- •Closure of the Peritoneum
- •Indications
- •Technique
- •Positioning
- •Pneumoperitoneum
- •Port Placement
- •Adhesiolysis
- •Measurement of the Hernia Defect
- •Placement of Mesh
- •Difficult Ventral or Incisional Hernias
- •Pain Following Laparoscopic Ventral or Incisional Hernia Repair
- •Preoperative Requirements and Workup
- •Patient Positioning
- •Port Placement
- •Surgical Anatomy
- •Surgical Principles
- •Technique
- •Division of the Short Gastric Vessels and Exposure of the Tail of the Pancreas
- •Division of the Hilar Vessels and Phrenic Attachments
- •Extraction of the Spleen in a Bag
- •Final Steps of the Procedure
- •Control of an Unnamed Vessel
- •Control of a Major Vessel
- •Splenic Injury
- •Maneuver of Last Resort During Bleeding of the Hilar Vessels
- •Distal Splenopancreatectomy
- •Selected Further Reading
- •13 Adrenalectomy
- •Principles
- •Patient Positioning
- •Technique
- •Immediate Postoperative Complications
- •Late Postoperative Complications
- •Laparoscopic Adjustable Band
- •Technique
- •Complications
- •Laparoscopic Sleeve Gastrectomy
- •Selected Further Reading
- •Laparoscopic Cholecystectomy
- •Laparoscopic Appendectomy
- •Laparoscopic Inguinal Hernia Repair
- •Selected Further Reading
- •Monitors
- •OR Table
- •Trocar Placement and Triangulation
- •Equipment
- •Needle Holders
- •Graspers
- •Suture Material
- •Intracorporeal Knot-Tying
- •Interrupted Stitch
- •Running Stitch
- •Pirouette
- •Extracorporeal Knot-Tying
- •Roeder’s Knot
- •Endoloop
- •Troubleshooting
- •Lost Needle
- •Short Suture
- •Subject Index

Appendectomy 7
OR Setup and Port Placement |
Acute |
The patient is placed in the supine position with the left arm or both arms tucked.A foley |
Appendicitis |
catheter is always placed as in other pelvic or lower abdominal procedures to decrease |
|
the risk of injury to the bladder during port placement. The surgeon and the assistant |
|
both stand on the left side of the patient facing the monitor located on the right side of |
|
the patient (Fig. 7.1). |
|
Pneumoperitoneum is created in the standard fashion using either the Hasson |
|
technique or a Veress needle. Care must be taken in patients who have had a longer |
|
course of disease if using a Veress needle, as the inflammation of the omentum and sur- |
|
rounding small bowel increase the risk of injury to the small bowel or other structures. |
|
The ports are inserted in an extended triangulation fashion. The laparoscope is |
|
placed at the umbilicus. Two 5 or 10 mm ports are inserted, one in the left lower quadrant |
|
in a position corresponding but opposite to McBurney’s point, and the second is placed |
|
in a suprapubic position. In a male patient, the right trocar is inserted in a position cor- |
|
responding to the left (Fig. 7.2a). In a female patient, both trocars can be hidden in the |
|
pubic hair line if cosmesis is an issue (Fig. 7.2b). If an additional trocar is needed for |
|
bowel retraction or suctioning, a 5-mm port can be placed in the right upper quadrant. |
|
Then the patient is placed in Trendelenburg position with the right side up. |
|
Care must be taken to avoid a “knitting needle” effect between instruments and the |
|
laparoscope; all ports should be placed in such a way that they have free movement and |
|
do not interfere with one another. The body habitus of the patient will influence place- |
|
ment of the ports to achieve this goal. |
|
N. Katkhouda, Advanced Laparoscopic Surgery,
DOI: 10.1007/978-3-540-74843-4_7, © Springer-Verlag Berlin Heidelberg 2011

120 |
Chapter 7 Appendectomy |
Fig. 7.1 Patient position for appendectomy. S surgeon; CA camera assistant
The surgeon’s left hand operates the Babcock grasper to retract the cecum or the tip of the appendix (if the appendix is in its usual paracecal position). The surgeon’s right hand operates a Kelly grasper to create windows in the mesoappendix. If the appendix is not clearly identifiable because it is retrocecal, the cecum needs to be mobilized and retracted medially (Fig. 7.3).
Acute Appendicitis |
121 |
a
b
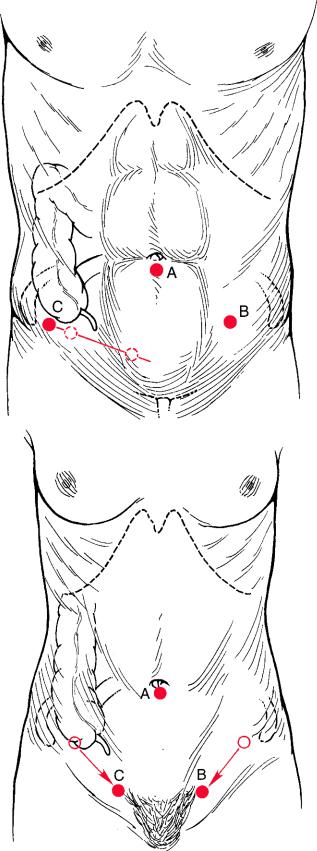
Fig. 7.2 Port positions for (a) a male patient and (b) a female patient. A telescope; B surgeon’s
right hand; C surgeon’s left hand
