
- •Vascular Surgery
- •SECTION AND BOARD OF VASCULAR SURGERY
- •Foreword to the First Edition
- •Preface to the First Edition
- •Preface to the Second Edition
- •Preface to the Third Edition
- •Contents
- •Contributors
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •1.1 Commentary
- •1.2 Beta-Adrenergic Antagonists
- •1.3 3-Hydroxy-3-Methylglutaryl Coenzyme A Reductase Inhibitors (Statins)
- •1.4 Percutaneous Revascularization
- •1.5 Coronary Artery Bypass Grafting
- •References
- •2: Abdominal Aortic Aneurysm
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •2.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •Question 12
- •Question 13
- •Question 14
- •3.1 Commentary
- •3.2 Case Analysis Quiz
- •References
- •4: Ruptured Abdominal Aortic Aneurysm
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •4.1 Commentary
- •References
- •5: Thoracoabdominal Aortic Aneurysm
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •5.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •Question 12
- •Question 13
- •6.1 Commentary
- •References
- •7: Aortic Dissection
- •7.1 Dissection: Stanford A
- •Question 1
- •Question 2
- •Question 3
- •7.2 Dissection: Stanford B
- •Question 4
- •Question 5
- •7.3 Commentary
- •References
- •8: Popliteal Artery Aneurysms
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •8.1 Popliteal Artery Aneurysm
- •References
- •9: Renal Artery Aneurysm
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •9.1 Commentary
- •References
- •10: Anastomotic Aneurysms
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •10.1 Commentary
- •10.2 Indications for Intervention
- •10.3 Treatment for Anastomotic Aneurysms
- •10.4 Infection in Anastomotic Aneurysms
- •10.5 Outcome
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •11.1 Commentary
- •References
- •12: Acute Thrombosis
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •12.1 Commentary
- •References
- •13: Arterial Embolism
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •13.1 Commentary
- •References
- •14: Blast Injury to the Lower Limb
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •14.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •15.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Smoking
- •Antiplatelet Agents
- •Blood Pressure (BP)
- •Glucose Status
- •Lipids
- •Emerging Risk Factors
- •Question 4
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •17.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •18.1 Commentary
- •18.2 Clinical Assessment
- •18.3 Imaging Techniques
- •18.4 Revascularization Options
- •18.5 Aortobifemoral Bypass
- •18.6 Iliac Angioplasty and Stenting
- •18.7 Iliac Stenting Combined with Profunda Femoris Artery Revascularization
- •18.8 Rationale for Angioplasty of “Donor” Iliac Artery Prior to Femorofemoral Crossover Bypass
- •18.10 Supervision and Follow-up of the Patient
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •Question 12
- •19.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •20.1 Commentary
- •References
- •21: Bypass to the Popliteal Artery
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •21.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •22.1 Commentary
- •References
- •23: Popliteal Artery Entrapment
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •23.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •24.1 Commentary
- •References
- •25: The Obturator Foramen Bypass
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •25.1 Commentary
- •25.2 Preoperative Measures
- •25.3 The Concept of the Obturator Foramen Bypass
- •25.4 Obturator Foramen Bypass Technique
- •References
- •26: Diabetic Foot
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •26.1 Commentary
- •References
- •27: Chronic Visceral Ischemia
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •27.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •28.1 Commentary
- •References
- •29: Renovascular Hypertension
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •29.1 Commentary
- •29.4 Intra-arterial Angiography
- •29.5 Duplex Ultrasonography (DU)
- •29.6 Treatment
- •29.6.1 Medical Treatment
- •29.6.2 Revascularization
- •29.7 Prognosis
- •References
- •30: Midaortic Syndrome
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •30.1 Commentary
- •References
- •31: Management of Portal Hypertension
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •31.1 Commentary
- •31.2 General Considerations
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •32.1 Commentary
- •References
- •33: The Carotid Body Tumor
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •33.1 Commentary
- •33.2 Clinical Presentation
- •33.3 Treatment
- •33.4 Summary
- •References
- •Question 1
- •Question 2
- •Question 3
- •34.1 Commentary
- •34.2 Vertebrobasilar Ischemia: Low-Flow Mechanism
- •Question 1
- •Question 2
- •34.3 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •35.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •36.1 Commentary
- •References
- •37: Acute Axillary/Subclavian Vein Thrombosis
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •37.1 Commentary
- •References
- •38: Raynaud’s Phenomenon
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •38.1 Commentary
- •References
- •39: Aortofemoral Graft Infection
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •39.1 Commentary
- •References
- •40: Aortoenteric Fistulas
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •40.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •41.1 Commentary
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Questions 7 and 8
- •Question 9
- •Question 10
- •Comment
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •42.1 Commentary
- •References
- •43: Amputations in an Ischemic Limb
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •43.1 Commentary
- •References
- •44: Congenital Vascular Malformation
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •44.1 Clinical Evaluation
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •44.2 Commentary
- •References
- •45: Klippel-Trenaunay Syndrome
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •45.1 Commentary
- •Clinical Presentation
- •Evaluation
- •Treatment
- •References
- •46: Deep Venous Thrombosis
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •46.1 Commentary
- •References
- •47: Endoluminal Ablation of Varicose Veins
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •47.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •48.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •50.1 Commentary
- •References
- •51: Iliofemoral Venous Thrombosis
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •50.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •52.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •53.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •54.1 Commentary
- •References
- •Index

|
|
Klippel-Trenaunay Syndrome |
45 |
|
|
Magdiel Trinidad-Hernandez and Peter Gloviczki |
|
|
|
A 38-year-old woman with the diagnosis of Klippel-Trenaunay Syndrome (KTS) presents with severe pain over venous malformations on the left thigh and severe hyperhidrosisoftheleftlegandfoot.Shehasahistoryofpulmonaryembolismatage 17. Otherwise, she is healthy and compliant with the use of compression garments. The diagnosis of KTS was made soon after birth because of the port wine stains, slightly larger and longer leg and lateral varicose veins of her left leg. Physical examinationshowsaportwinenevusontheleftbuttockwithvaricoseveinsandsofttissue hypertrophy along the anterolateral aspect of the left leg and thigh. These areas are tender to palpation and leg elevation eases their appearance. Hyperhidrosis behind the knee and dorsum of the foot and in the interdigital spaces is obvious. Limb length discrepancy is 1 cm. The remainder of the exam is unremarkable.
Question 1
Which of the following is not a characteristic finding in patients with KTS?
A. High-flow arteriovenous shunting B. Long bone hypertrophy
C. Lateral varicosity D. Port wine nevus
No bruits or thrills were detected during the physical examination. If arteriovenous shunting is suspected further studies should be performed to characterize the anomaly. These include segmental limb pressures and ankle-brachial indices.
P. Gloviczki ( )
Division of Vascular and Endovascular Surgery,
Gonda Vascular Center, Mayo Clinic, Rochester, MN, USA
G. Geroulakos and B. Sumpio (eds.), Vascular Surgery, |
473 |
DOI: 10.1007/978-1-84996-356-5_45, © Springer-Verlag London Limited 2011 |
|

474 |
M. Trinidad-Hernandez and P. Gloviczki |
|
|
Question 2
The patient’s pain is affecting her quality of life and she seeks surgical treatment. What conditions should be present prior to offering any type of surgical procedure?
A. Duplex ultrasound showing valvular incompetence and absence of DVT B. Patent deep venous system
C. Sufficient collateral circulation
D. Outflow plethysmography without evidence of venous obstruction
The patient underwent a complete venous duplex ultrasound with valvular competence evaluation and magnetic resonance venography (MRV) (Fig. 45.1a and b). The deep venous system was found to be patent. Only mild left popliteal vein incompetence was encountered. The MRV confirms a patent and normal deep venous system. A large lateral vein perforates the fascia and gives rise to multiple varicosities in the lower thigh.
a
b
Fig. 45.1 (a) Magnetic resonance venography of the left thigh demonstrates low flow venous malformation of the lateral left thigh. There is a dilated lateral superficial vein and a dilated profunda femoris vein visible. Soft tissue hypertrophy are present in the lateral portion of the thigh. (b) A large lateral perforator vein is connected to multiple congenital varicose veins in the distal thigh

45 Klippel-Trenaunay Syndrome |
475 |
|
|
Question 3
What treatment options are suitable for this patient?
A. Vein stripping and phlebectomy B. Endovenous closure
C. Sclerotherapy
D. Lumbar sympathectomy
Thepatientunderwentlumbarsympathectomy,atemporaryIVCfilterplacement,andambulatoryphlebectomywithligationoftheperforatingembryonicveinandavulsionandexcision of varicose veins and venous malformations of the left leg. There was no long lateral vein for treatmentwithendovenousclosure.Theoperationwasuneventful.Thehyperhidrosisresolved and the limb swelling and pain improved. She continues to wear compression garments.
A 13-year-old boy with KTS presents for follow-up. He was first evaluated at 6 years of age when the diagnosis was made. Since then, he has been managed conservatively with elastic compression stockings. He has a prominent lateral vein with varicose veins of the right lateral leg and thigh. There are venular blebs in the lateral leg that occasionally bleed. There is a 1.5 cm limb discrepancy. He has never had cellulitis nor has he suffered thromboembolism. Otherwise, he is healthy. The patient is seeking surgical treatment for his varicose veins.
Question 4
What are the indications for treatment in patients with KTS?
A. Bleeding
B. Refractory venous ulcers C. Soft tissue infection D. Acute thromboembolism
Although the patient has not developed venous ulcers, infection or thromboembolism he has suffered from mild bleeding episodes and has significant pain. He is a candidate for varicose vein surgery.
Question 5
What tests should be performed to evaluate this patient prior to surgical intervention?
A. Outflow plethysmography and exercise plethysmography (calf muscle pump function) with and without thigh tourniquets
B. MRV
476 |
M. Trinidad-Hernandez and P. Gloviczki |
|
|
a |
b |
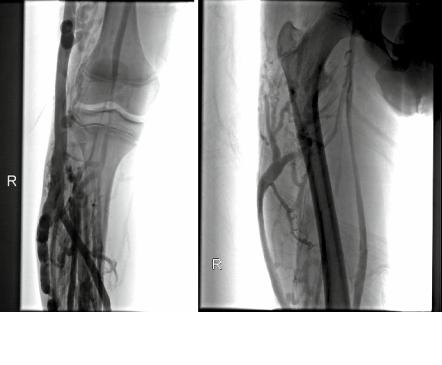
Fig. 45.2 (a) Ascending venogram demonstrates large lateral embryonic vein connected to multiple incompetent perforating veins in the right leg. The popliteal vein appears to be hypoplastic.(b) The lateral embryonic vein drains into the deep femoral vein
C. Ascending venogram D. Duplex scanning
Ascendingvenogramdemonstratesalargeanddistendedlateralembryonicveinarisingfrom multiple perforators in the leg and draining into the deep femoral vein (Fig. 45.2a and b). The paired popliteal veins are hypoplastic.
Question 6
What are the expected findings in outflow plethysmography?
A. The application of a tourniquet will decrease venous outflow.
B. The application of a tourniquet will have minimal effect on venous outflow. C. Tourniquet use will not be helpful for the evaluation of this patient.
Outflow plethysmography demonstrated moderate right side venous obstruction in this patient. However, when a tourniquet was applied to the thigh and below the knee the venous outflow became severely obstructed (Fig. 45.3). This is strong evidence that the superficial veins are the primary route of venous drainage in the right limb.
