
- •Vascular Surgery
- •SECTION AND BOARD OF VASCULAR SURGERY
- •Foreword to the First Edition
- •Preface to the First Edition
- •Preface to the Second Edition
- •Preface to the Third Edition
- •Contents
- •Contributors
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •1.1 Commentary
- •1.2 Beta-Adrenergic Antagonists
- •1.3 3-Hydroxy-3-Methylglutaryl Coenzyme A Reductase Inhibitors (Statins)
- •1.4 Percutaneous Revascularization
- •1.5 Coronary Artery Bypass Grafting
- •References
- •2: Abdominal Aortic Aneurysm
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •2.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •Question 12
- •Question 13
- •Question 14
- •3.1 Commentary
- •3.2 Case Analysis Quiz
- •References
- •4: Ruptured Abdominal Aortic Aneurysm
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •4.1 Commentary
- •References
- •5: Thoracoabdominal Aortic Aneurysm
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •5.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •Question 12
- •Question 13
- •6.1 Commentary
- •References
- •7: Aortic Dissection
- •7.1 Dissection: Stanford A
- •Question 1
- •Question 2
- •Question 3
- •7.2 Dissection: Stanford B
- •Question 4
- •Question 5
- •7.3 Commentary
- •References
- •8: Popliteal Artery Aneurysms
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •8.1 Popliteal Artery Aneurysm
- •References
- •9: Renal Artery Aneurysm
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •9.1 Commentary
- •References
- •10: Anastomotic Aneurysms
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •10.1 Commentary
- •10.2 Indications for Intervention
- •10.3 Treatment for Anastomotic Aneurysms
- •10.4 Infection in Anastomotic Aneurysms
- •10.5 Outcome
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •11.1 Commentary
- •References
- •12: Acute Thrombosis
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •12.1 Commentary
- •References
- •13: Arterial Embolism
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •13.1 Commentary
- •References
- •14: Blast Injury to the Lower Limb
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •14.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •15.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Smoking
- •Antiplatelet Agents
- •Blood Pressure (BP)
- •Glucose Status
- •Lipids
- •Emerging Risk Factors
- •Question 4
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •17.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •18.1 Commentary
- •18.2 Clinical Assessment
- •18.3 Imaging Techniques
- •18.4 Revascularization Options
- •18.5 Aortobifemoral Bypass
- •18.6 Iliac Angioplasty and Stenting
- •18.7 Iliac Stenting Combined with Profunda Femoris Artery Revascularization
- •18.8 Rationale for Angioplasty of “Donor” Iliac Artery Prior to Femorofemoral Crossover Bypass
- •18.10 Supervision and Follow-up of the Patient
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •Question 12
- •19.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •20.1 Commentary
- •References
- •21: Bypass to the Popliteal Artery
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •21.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •22.1 Commentary
- •References
- •23: Popliteal Artery Entrapment
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •23.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •24.1 Commentary
- •References
- •25: The Obturator Foramen Bypass
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •25.1 Commentary
- •25.2 Preoperative Measures
- •25.3 The Concept of the Obturator Foramen Bypass
- •25.4 Obturator Foramen Bypass Technique
- •References
- •26: Diabetic Foot
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •26.1 Commentary
- •References
- •27: Chronic Visceral Ischemia
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •27.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •28.1 Commentary
- •References
- •29: Renovascular Hypertension
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •29.1 Commentary
- •29.4 Intra-arterial Angiography
- •29.5 Duplex Ultrasonography (DU)
- •29.6 Treatment
- •29.6.1 Medical Treatment
- •29.6.2 Revascularization
- •29.7 Prognosis
- •References
- •30: Midaortic Syndrome
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •30.1 Commentary
- •References
- •31: Management of Portal Hypertension
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •31.1 Commentary
- •31.2 General Considerations
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •32.1 Commentary
- •References
- •33: The Carotid Body Tumor
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •33.1 Commentary
- •33.2 Clinical Presentation
- •33.3 Treatment
- •33.4 Summary
- •References
- •Question 1
- •Question 2
- •Question 3
- •34.1 Commentary
- •34.2 Vertebrobasilar Ischemia: Low-Flow Mechanism
- •Question 1
- •Question 2
- •34.3 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •35.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •36.1 Commentary
- •References
- •37: Acute Axillary/Subclavian Vein Thrombosis
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •37.1 Commentary
- •References
- •38: Raynaud’s Phenomenon
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •38.1 Commentary
- •References
- •39: Aortofemoral Graft Infection
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •39.1 Commentary
- •References
- •40: Aortoenteric Fistulas
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •40.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •41.1 Commentary
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Questions 7 and 8
- •Question 9
- •Question 10
- •Comment
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •42.1 Commentary
- •References
- •43: Amputations in an Ischemic Limb
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •43.1 Commentary
- •References
- •44: Congenital Vascular Malformation
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •44.1 Clinical Evaluation
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •44.2 Commentary
- •References
- •45: Klippel-Trenaunay Syndrome
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •45.1 Commentary
- •Clinical Presentation
- •Evaluation
- •Treatment
- •References
- •46: Deep Venous Thrombosis
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •46.1 Commentary
- •References
- •47: Endoluminal Ablation of Varicose Veins
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •47.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •48.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •50.1 Commentary
- •References
- •51: Iliofemoral Venous Thrombosis
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •50.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •Question 11
- •52.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •Question 6
- •Question 7
- •Question 8
- •Question 9
- •Question 10
- •53.1 Commentary
- •References
- •Question 1
- •Question 2
- •Question 3
- •Question 4
- •Question 5
- •54.1 Commentary
- •References
- •Index

|
|
Amputations in an Ischemic Limb |
43 |
|
|
Kenneth R. Ziegler and Bauer Sumpio |
|
|
|
A 70 year old white male hospitalized for pneumonia is discovered to have a Stage IV heel ulcer on his left foot by the nursing staff. The patient describes no pain at the site of the ulcer, and has no previous history of sores on his lower extremities. He denies a history of diabetes, but states that he has been having progressive difficulty lately in walking distances due to cramps in his calves bilaterally. His past medical history is significant for hypertension and stable angina, for which he takes nitrates and a beta-blocker. His only previous surgery was a right inguinal herniorrhaphy 30 years ago. He admits to a 50 pack-year tobacco history, and still smokes.
The ulcer appears to have a dark base on examination, with mild malodorous discharge. His heart rate is 84 bpm, blood pressure is 140/70 mmHg, and he is afebrile on examination. He is alert, awake, and normally conversant, but states that his prolonged bedrest has reduced his normal willingness to get out of bed and ambulate.
Question 1
The most common cause of major lower extremity amputation in the United States is:
A. Trauma
B. Complications secondary to diabetes mellitus C. Neoplasm
D. Acute limb ischemia
E. Vascular bypass graft failure
Physical examination reveals that the femoral and popliteal pulses are palpable bilaterally, but the pedal pulses are absent. Doppler exam reveals a faintly monophasic dorsalis pedis (DP) signal and absent posterior tibital (PT) signal on the left foot, while biphasic signals are present at the DP and PT on the right. Bedside pressure exams reveal an ankle-brachial index of 0.2 on the left, 0.5 on the right.
B. Sumpio ( )
Department of Surgery, School of Medicine, Yale University, New Haven, CT, USA
G. Geroulakos and B. Sumpio (eds.), Vascular Surgery, |
441 |
DOI: 10.1007/978-1-84996-356-5_43, © Springer-Verlag London Limited 2011 |
|

442 |
K.R. Ziegler and B. Sumpio |
|
|
|
|
Fig. 43.1 (a) Left heel ulcer |
a |
|
after uncapping of eschar and |
||
|
||
debridement of nonviable |
|
|
tissues. Note the pink base of |
|
|
the ulcer with backbleeding |
|
|
from the wound bed. (b) |
|
|
Plain film of the left foot. |
|
|
The radiolucency of the left |
|
|
heel reflects the ulcerated |
|
|
tissue; no appreciable |
|
|
osteomyelitis is evident. |
|
b
The eschar on the ulcer is uncapped, and the remainder of the wound is debrided (Fig. 43.1). Tissue samples and swabs are sent for bacterial culture and sensitivity assays. A CT angiogram is ordered for the patient.
Question 2
In anticipating the results of the angiogram, what is true about primary and secondary amputation in the treatment of chronic limb ischemia?
A. Primary amputation is the most common form of initial therapy in the treatment of chronic limb ischemia.
B. Overwhelming infection is the most common cause of secondary amputation.
C. Early graft occlusion always results in a secondary amputation within the first year after arterial reconstruction.
D. Primary amputation is indicated when extensive gangrene has compromised the foot to such a degree that it cannot be salvaged.
E. All of the above. F. None of the above.
43 Amputations in an Ischemic Limb |
443 |
|
|
Question 3
If the results of the angiogram preclude vascular reconstruction and the wound remains non-healing, which of the following would be the single best non-invasive method to determine the level of appropriate amputation?
A. Pulse volume recordings/segmental systolic blood pressure measurements. B. Transcutaneous oxygen pressure measurements.
C. Skin fluorescein uptake/radiotracer injection. D. Skin thermography.
E. Clinical assessment of popliteal pulses, skin temperature, dependent rubor. F. There is no test that can reliably predict primary healing by itself.
While awaiting angiography, the Vascular Surgery resident is alerted to a sudden deterioration in the patient’s condition. The patient has become febrile, hypotensive, and tachycardic. He is awake, but delirious. Examination of the left foot reveals frank purulence from the wound, expressible with manual pressure on the dorsal forefoot. The Achilles tendon appears grossly infected with extensive loss of structural integrity. There is no crepitance on palpation.
Question 4
Which of the following is the most appropriate initial intervention at this time?
A. IV antibiotics and medical management alone
B. IV antibiotics, below-the-knee amputation (BKA) with flap (non-staged)
C. IV antibiotics, ankle disarticulation in expectation of a staged BKA or above-the-knee amputation (AKA)
D. IV antibiotics, immediate above-the-knee amputation E. IV antibiotics, debridement, and vascular reconstruction
The patient is started on broad spectrum IV antibiotics and is taken urgently to the operating room for an ankle disarticulation under general anesthesia. He is extubated post-oper- atively after an initial stay in the ICU for resuscitation and recovers from sepsis adequately on the surgery ward. The amputated stump appears to be draining adequately without signs of expanding cellulitis. One week later, he returns to the operating room for his staged amputation.
Question 5
Which of the following is true regarding the relative advantages and disadvantages of a below-the-knee amputation as compared to an above-the-knee amputation in elderly patients?
A. Most patients who undergo unilateral AKA do not achieve independent ambulation. B. PatientswhoundergoBKAexperiencea10–40%increaseinenergyexpenditureabove
their normal baseline when ambulating.
444 |
K.R. Ziegler and B. Sumpio |
|
|
C. Proximal amputations are associated with a higher probability of primary healing. D. The rehabilitative advantages of BKA over AKA are negligible in patients who are
unable to ambulate due to their comorbid conditions. E. All of the above.
Question 6
Which of the following factors and complications are NOT associated with below-knee stump failure necessitating revision and/or a more proximal amputation?
A. Intrinsic wound infection/sepsis B. Trauma to the residual limb C. Wound edge necrosis/ischemia D. Stump ulceration
E. Early ambulation and weight-bearing on the stump
Question 7
Advantages of a customizable removable immediate postoperative prosthesic after BKA include which of the following?
A. Rigid support to control or prevent joint flexion contracture B. Accelerated wound healing and stump maturation
C. Minimizing postsurgical edema and pain
D. Decreasing inactivity by assisting in early ambulation E. Decreased need for postoperative follow-up
F. Protection from trauma
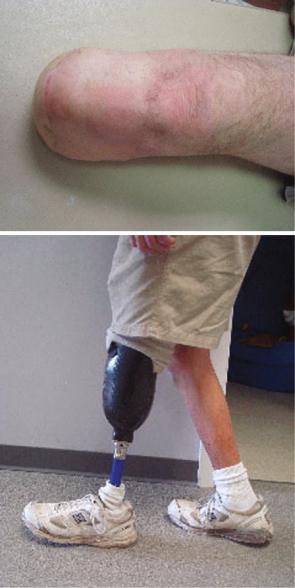
The patient recovers well on the vascular ward post-operatively. His wounds appear to be healing well without signs of infection (Fig. 43.2a); his pain is well-managed on oral narcotics, but he states that he has reduced sensation on the skin over his residual limb. He begins physical therapy in the hospital, but has initial resistance to getting out of bed due to deconditioning. Though he makes significant progress toward walking while in the hospital, he is discharged to a short-term rehabilitation facility after consultation with the physical and occupational therapy team (Fig. 43.2b).
Question 8
Whichofthefollowingstatementsregardingthepost-operativecareofamputationpatients is false?
A. For optimal patient recovery, a combination of good amputation level selection and early ambulation rehabilitation is necessary.
B. The patient is best treated by a multidisciplinary team that includes the vascular surgeon, a prosthetist, physical therapy, and mental health professionals as warranted.
43 Amputations in an Ischemic Limb |
445 |
|
|
Fig. 43.2 The patient at his post-discharge clinic follow-up appointment. (a) The well-healed left BKA stump without complications. (b) The patient demonstrating independent ambulation with his BK prosthesis
a
b
C. The 5 year life expectancy of diabetic patients is less than 50% after major lower extremity amputation.
D. Patient education and contralateral foot care are key for continued patient well-being. E. Elderly patients commonly ambulate after bilateral above-knee amputations.
