
- •Foreword
- •Preface
- •Contents
- •About the Editors
- •Contributors
- •1: Tracheobronchial Anatomy
- •Trachea
- •Introduction
- •External Morphology
- •Internal Morphology
- •Mucous Layer
- •Blood Supply
- •Anatomo-Clinical Relationships
- •Bronchi
- •Main Bronchi
- •Bronchial Division
- •Left Main Bronchus (LMB)
- •Right Main Bronchus (RMB)
- •Blood Supply
- •References
- •2: Flexible Bronchoscopy
- •Introduction
- •History
- •Description
- •Indications and Contraindications
- •Absolute Contraindications
- •Procedure Preparation
- •Technique of FB Procedure
- •Complications of FB Procedure
- •Basic Diagnostic Procedures
- •Bronchoalveolar Lavage (BAL)
- •Transbronchial Lung Biopsy (TBLB)
- •Transbronchial Needle Aspiration (TBNA)
- •Bronchial Brushings
- •Advanced Diagnostic Bronchoscopy
- •EBUS-TBNA
- •Ultrathin Bronchoscopy
- •Transbronchial Lung Cryobiobsy (TBLC)
- •Therapeutic Procedures Via FB
- •LASER Bronchoscopy
- •Electrocautery
- •Argon Plasma Coagulation (APC)
- •Cryotherapy
- •Photodynamic Therapy
- •Airway Stent Placement
- •Endobronchial Valve Placement
- •Conclusion
- •References
- •History and Historical Perspective
- •Indications and Contraindications
- •Procedure Description
- •Procedure Planning
- •Target Approximation
- •Sampling
- •Complications
- •Future Directions
- •Summary and Recommendations
- •References
- •4: Rigid Broncoscopy
- •Innovations
- •Ancillary Equipment
- •Rigid Bronchoscopy Applications
- •Laser Bronchoscopy
- •Tracheobronchial Prosthesis
- •Transbronchial Needle Aspiration (TBNA)
- •Rigid Bronchoscope in Other Treatments for Bronchial Obstruction
- •Mechanical Debridement
- •Pediatric Rigid Bronchoscopy
- •Tracheobronchial Dilatation
- •Foreign Bodies Removal
- •Other Indications
- •Complications
- •The Procedure
- •Some Conclusions
- •References
- •History and Historical Perspective
- •Indications and Contraindications
- •Preprocedural Evaluation and Preparation
- •Physical Examination
- •Procedure-Related Indications
- •Application of the Technique
- •Topical Anesthesia
- •Anesthesia of the Nasal Mucosa and Nasopharynx
- •Anesthesia of the Mouth and Oropharynx
- •Superior Laryngeal Nerve Block
- •Recurrent Laryngeal Nerve Block (RLN)
- •Conscious Sedation
- •Monitored Anesthesia Care (MAC)
- •General Anesthesia
- •Monitoring the Depth of Anesthesia
- •Interventional Bronchoscopy Suites
- •Airway Devices
- •Laryngeal Mask Airway (LMA)
- •Endotracheal Tube (ETT)
- •Rigid Bronchoscope
- •Modes of Ventilation
- •Spontaneous Ventilation
- •Assisted Ventilation
- •Noninvasive Positive Pressure Ventilation (NIV)
- •Positive Pressure Controlled Mechanical Ventilation
- •Jet Ventilation
- •Electronic Mechanical Jet Ventilation
- •Postprocedure Care
- •Special Consideration
- •Anesthesia for Peripheral Diagnostic and Therapeutic Bronchoscopy
- •Anesthesia for Interventional Bronchoscopic Procedures During the COVID-19 Pandemic
- •Summary and Recommendations
- •Conclusion
- •References
- •Background
- •Curricular Structure and Delivery
- •What Is a Bronchoscopy Curriculum?
- •Tradition, Teaching Styles, and Beliefs
- •Using Assessment Tools to Guide the Educational Process
- •The Ethics of Teaching
- •When Learners Teach: The Journey from Novice to Mastery and Back Again
- •The Future Is Now
- •References
- •Interventional Procedure
- •Assessment of Flow–Volume Curve
- •Dyspnea
- •Analysis of Pressure–Pressure Curve
- •Conclusions
- •References
- •Introduction
- •Adaptations of the IP Department
- •Environmental Control
- •Personal Protective Equipment
- •Procedure Performance
- •Bronchoscopy in Intubated Patients
- •Other Procedures in IP Unit
- •References
- •Introduction
- •Safety
- •Patient Safety
- •Provider Safety
- •Patient Selection and Screening
- •Lung Cancer Diagnosis and Staging
- •Inpatients
- •COVID-19 Clearance
- •COVID Clearance: A Role for Bronchoscopy
- •Long COVID: A Role for Bronchoscopy
- •Preparing for the Next Pandemic
- •References
- •Historical Perspective
- •Indications and Contraindications
- •Evidence-Based Review
- •Summary and Recommendations
- •References
- •Introduction
- •Clinical Presentation
- •Diagnosis
- •Treatment
- •History and Historical Perspectives
- •Indications and Contraindications
- •Benign and Malignant Tumors
- •Tumors with Uncertain Prognosis
- •Application of the Technique
- •Evidence Based Review
- •Summary and Recommendations
- •References
- •12: Cryotherapy and Cryospray
- •Introduction
- •Historical Perspective
- •Equipment
- •Cryoadhesion
- •Indications
- •Cryorecanalization
- •Cryoadhesion and Foreign Body Removal
- •Cryoadhesion and Mucus Plugs/Blood Clot Retrieval
- •Endobronchial Cryobiopsy
- •Transbronchial Cryobiopsy for Lung Cancer
- •Safety Concerns and Contraindications
- •Cryoablation
- •Indications
- •Evidence
- •Safety Concerns and Contraindications
- •Cryospray
- •Indications
- •Evidence
- •Safety Concerns and Contraindications
- •Advantages of Cryotherapy
- •Limitations
- •Future Research Directions
- •References
- •13: Brachytherapy
- •History and Historical Perspective
- •Indications and Contraindications
- •Application of the Technique
- •Evidence-Based Review
- •Adjuvant Treatment
- •Palliative Treatment
- •Complications
- •Summary and Recommendations
- •References
- •14: Photodynamic Therapy
- •Introduction
- •Photosensitizers
- •First-Generation Photosensitizers
- •M-Tetrahidroxofenil Cloro (mTHPC) (Foscan®)
- •PDT Reaction
- •Tumor Damage Process
- •Procedure
- •Indications
- •Curative PDT Indications
- •Palliative PDT Indications
- •Contraindications
- •Rationale for Use in Early-Stage Lung Cancer
- •Rationale
- •PDT in Combination with Other Techniques for Advanced-Stage Non-small Cell Lung Cancer
- •Commentary
- •Complementary Endoscopic Methods for PDT Applications
- •New Perspectives
- •Other PDT Applications
- •Conclusions
- •References
- •15: Benign Airways Stenosis
- •Etiology
- •Congenital Tracheal Stenosis
- •Iatrogenic
- •Infectious
- •Idiopathic Tracheal Stenosis
- •Distal Bronchial Stenosis
- •Diagnosis Methods
- •Patient History
- •Imaging Techniques
- •Bronchoscopy
- •Pulmonary Function Test
- •Treatment
- •Endoscopic Treatment
- •Dilatation
- •Laser Therapy
- •Stents
- •How to Proceed
- •Stent Placement
- •Placing a Montgomery T Tube
- •The Rule of Twos for Benign Tracheal Stenosis (Fig. 15.23)
- •Surgery
- •Summary and Recommendations
- •References
- •16: Endobronchial Prostheses
- •Introduction
- •Indications
- •Extrinsic Compression
- •Intraluminal Obstruction
- •Stump Fistulas
- •Esophago-respiratory Fistulas (ERF)
- •Expiratory Central Airway Collapse
- •Physiologic Rationale for Airway Stent Insertion
- •Stent Selection Criteria
- •Stent-Related Complications
- •Granulation Tissue
- •Stent Fracture
- •Migration
- •Contraindications
- •Follow-Up and Patient Education
- •References
- •Introduction
- •Overdiagnosis
- •False Positives
- •Radiation
- •Risk of Complications
- •Lung Cancer Screening Around the World
- •Incidental Lung Nodules
- •Management of Lung Nodules
- •References
- •Introduction
- •Minimally Invasive Procedures
- •Mediastinoscopy
- •CT-Guided Transthoracic Biopsy
- •Fluoroscopy-Guided Transthoracic Biopsies
- •US-Guided Transthoracic Biopsy
- •Thoracentesis and Pleural Biopsy
- •Thoracentesis
- •Pleural Biopsy
- •Surgical or Medical Thoracoscopy
- •Image-Guided Pleural Biopsy
- •Closed Pleural Biopsy
- •Image-Guided Biopsies for Extrathoracic Metastases
- •Tissue Acquisition, Handling and Processing
- •Implications of Tissue Acquisition
- •Guideline Recommendations for Tissue Acquisition in Mediastinal Staging
- •Methods to Overcome Challenges in Tissue Acquisition and Genotyping
- •Rapid on-Site Evaluation (ROSE)
- •Sensitive Genotyping Assays
- •Liquid Biopsy
- •Summary, Recommendations and Highlights
- •References
- •History
- •Data Source and Methodology
- •Tumor Size
- •Involvement of the Main Bronchus
- •Atelectasis/Pneumonitis
- •Nodal Staging
- •Proposal for the Revision of Stage Groupings
- •Small Cell Lung Cancer (SCLC)
- •Discussion
- •Methodology
- •T Descriptors
- •N Descriptors
- •M Descriptors
- •Summary
- •References
- •Introduction
- •Historical Perspective
- •Fluoroscopy
- •Radial EBUS Mini Probe (rEBUS)
- •Ultrasound Bronchoscope (EBUS)
- •Virtual Bronchoscopy
- •Trans-Parenchymal Access
- •Cone Beam CT (CBCT)
- •Lung Vision
- •Sampling Instruments
- •Conclusions
- •References
- •History and Historical Perspective
- •Narrow Band Imaging (NBI)
- •Dual Red Imaging (DRI)
- •Endobronchial Ultrasound (EBUS)
- •Optical Coherence Tomography (OCT)
- •Indications and Contraindications
- •Confocal Laser Endomicroscopy and Endocytoscopy
- •Raman Spectrophotometry
- •Application of the Technique
- •Supplemental Technology for Diagnostic Bronchoscopy
- •Evidence-Based Review
- •Summary and Recommendations, Highlight of the Developments During the Last Three Years (2013 on)
- •References
- •Introduction
- •History and Historical Perspective
- •Endoscopic AF-OCT System
- •Preclinical Studies
- •Clinical Studies
- •Lung Cancer
- •Asthma
- •Airway and Lumen Calibration
- •Obstructive Sleep Apnea
- •Future Applications
- •Summary
- •References
- •23: Endobronchial Ultrasound
- •History and Historical Perspective
- •Equipment
- •Technique
- •Indication, Application, and Evidence
- •Convex Probe Ultrasound
- •Equipment
- •Technique
- •Indication, Application, and Evidence
- •CP-EBUS for Malignant Mediastinal or Hilar Adenopathy
- •CP-EBUS for the Staging of Non-small Cell Lung Cancer
- •CP-EBUS for Restaging NSCLC After Neoadjuvant Chemotherapy
- •Complications
- •Summary
- •References
- •Introduction
- •What Is Electromagnetic Navigation?
- •SuperDimension Navigation System (EMN-SD)
- •Computerized Tomography
- •Computer Interphase
- •The Edge Catheter: Extended Working Channel (EWC)
- •Procedural Steps
- •Planning
- •Detecting Anatomical Landmarks
- •Pathway Planning
- •Saving the Plan and Exiting
- •Registration
- •Real-Time Navigation
- •SPiN System Veran Medical Technologies (EMN-VM)
- •Procedure
- •Planning
- •Navigation
- •Biopsy
- •Complications
- •Limitations
- •Summary
- •References
- •Introduction
- •Image Acquisition
- •Hardware
- •Practical Considerations
- •Radiation Dose
- •Mobile CT Studies
- •Future Directions
- •Conclusion
- •References
- •26: Robotic Assisted Bronchoscopy
- •Historical Perspective
- •Evidence-Based Review
- •Diagnostic Yield
- •Monarch RAB
- •Ion Endoluminal Robotic System
- •Summary
- •References
- •History and Historical Perspective
- •Indications and Contraindications
- •General
- •Application of the Technique
- •Preoperative Care
- •Patient’s Position and Operative Field
- •Incision and Initial Dissection
- •Palpation
- •Biopsy
- •Control of Haemostasis and Closure
- •Postoperative Care
- •Complications
- •Technical Variants
- •Extended Cervical Mediastinoscopy
- •Mediastinoscopic Biopsy of Scalene Lymph Nodes
- •Inferior Mediastinoscopy
- •Mediastino-Thoracoscopy
- •Video-Assisted Mediastinoscopic Lymphadenectomy
- •Transcervical Extended Mediastinal Lymphadenectomy
- •Evidence-Based Review
- •Summary and Recommendations
- •References
- •Introduction
- •Case 1
- •Adrenal and Hepatic Metastases
- •Brain
- •Bone
- •Case 1 Continued
- •Biomarkers
- •Case 1 Concluded
- •Case 2
- •Chest X-Ray
- •Computerized Tomography
- •Positive Emission Tomography
- •Magnetic Resonance Imaging
- •Endobronchial Ultrasound with Transbronchial Needle Aspiration
- •Transthoracic Needle Aspiration
- •Transbronchial Needle Aspiration
- •Endoscopic Ultrasound with Needle Aspiration
- •Combined EUS-FNA and EBUS-TBNA
- •Case 2 Concluded
- •Case 3
- •Standard Cervical Mediastinoscopy
- •Extended Cervical Mediastinoscopy
- •Anterior Mediastinoscopy
- •Video-Assisted Thoracic Surgery
- •Case 3 Concluded
- •Case 4
- •Summary
- •References
- •29: Pleural Anatomy
- •Pleural Embryonic Development
- •Pleural Histology
- •Cytological Characteristics
- •Mesothelial Cells Functions
- •Pleural Space Defense Mechanism
- •Pleura Macroscopic Anatomy
- •Visceral Pleura (Pleura Visceralis or Pulmonalis)
- •Parietal Pleura (Pleura Parietalis)
- •Costal Parietal Pleura (Costalis)
- •Pleural Cavity (Cavitas Thoracis)
- •Pleural Apex or Superior Pleural Sinus [12–15]
- •Anterior Costal-Phrenic Sinus or Cardio-Phrenic Sinus
- •Posterior Costal-Phrenic Sinus
- •Cost-Diaphragmatic Sinus or Lateral Cost-Phrenic Sinus
- •Fissures18
- •Pleural Vascularization
- •Parietal Pleura Lymphatic Drainage
- •Visceral Pleura Lymphatic Drainage
- •Pleural Innervation
- •References
- •30: Chest Ultrasound
- •Introduction
- •The Technique
- •The Normal Thorax
- •Chest Wall Pathology
- •Pleural Pathology
- •Pleural Thickening
- •Pneumothorax
- •Pulmonary Pathology
- •Extrathoracic Lymph Nodes
- •COVID and Chest Ultrasound
- •Conclusions
- •References
- •Introduction
- •History of Chest Tubes
- •Overview of Chest Tubes
- •Contraindications for Chest Tube Placement
- •Chest Tube Procedural Technique
- •Special Considerations
- •Pneumothorax
- •Empyema
- •Hemothorax
- •Chest Tube Size Considerations
- •Pleural Drainage Systems
- •History of and Introduction to Indwelling Pleural Catheters
- •Indications and Contraindications for IPC Placement
- •Special Considerations
- •Non-expandable Lung
- •Chylothorax
- •Pleurodesis
- •Follow-Up and IPC Removal
- •IPC-Related Complications and Management
- •Competency and Training
- •Summary
- •References
- •32: Empyema Thoracis
- •Historical Perspectives
- •Incidence
- •Epidemiology
- •Pathogenesis
- •Clinical Presentation
- •Radiologic Evaluation
- •Biochemical Analysis
- •Microbiology
- •Non-operative Management
- •Prognostication
- •Surgical Management
- •Survivorship
- •Summary and Recommendations
- •References
- •Evaluation
- •Initial Intervention
- •Pleural Interventions for Recurrent Symptomatic MPE
- •Especial Circumstances
- •References
- •34: Medical Thoracoscopy
- •Introduction
- •Diagnostic Indications for Medical Thoracoscopy
- •Lung Cancer
- •Mesothelioma
- •Other Tumors
- •Tuberculosis
- •Therapeutic Indications
- •Pleurodesis of Pneumothorax
- •Thoracoscopic Drainage
- •Drug Delivery
- •Procedural Safety and Contraindications
- •Equipment
- •Procedure
- •Pre-procedural Preparations and Considerations
- •Procedural Technique [32]
- •Medical Thoracoscopy Versus VATS
- •Conclusion
- •References
- •Historical Perspective
- •Indications and Contraindications
- •Evidence-Based Review
- •Endobronchial Valves
- •Airway Bypass Tracts
- •Coils
- •Other Methods of ELVR
- •Summary and Recommendations
- •References
- •36: Bronchial Thermoplasty
- •Introduction
- •Mechanism of Action
- •Trials
- •Long Term: Ten-Year Study
- •Patient Selection
- •Bronchial Thermoplasty Procedure
- •Equipment
- •Pre-procedure
- •Bronchoscopy
- •Post-procedure
- •Conclusion
- •References
- •Introduction
- •Bronchoalveolar Lavage (BAL)
- •Technical Aspects of BAL Procedure
- •ILD Cell Patterns and Diagnosis from BAL
- •Technical Advises for Conventional TLB and TLB-C in ILD
- •Future Directions
- •References
- •Introduction
- •The Pediatric Airway
- •Advanced Diagnostic Procedures
- •Endobronchial Ultrasound
- •Virtual Navigational Bronchoscopy
- •Cryobiopsy
- •Therapeutic Procedures
- •Dilation Procedures
- •Thermal Techniques
- •Mechanical Debridement
- •Endobronchial Airway Stents
- •Metallic Stents
- •Silastic Stents
- •Novel Stents
- •Endobronchial Valves
- •Bronchial Thermoplasty
- •Discussion
- •References
- •Introduction
- •Etiology
- •Congenital ADF
- •Malignant ADF
- •Cancer Treatment-Related ADF
- •Benign ADF
- •Iatrogenic ADF
- •Diagnosis
- •Treatment Options
- •Endoscopic Techniques
- •Stents
- •Clinical Results
- •Stent Complications
- •Other Available Stents
- •Other Endoscopic Methods
- •References
- •Introduction
- •Anatomy and Physiology of Swallowing
- •Functional Physiology of Swallowing
- •Epidemiology and Risk Factors
- •Types of Foreign Bodies
- •Organic
- •Inorganic
- •Mineral
- •Miscellaneous
- •Clinical Presentation
- •Acute FB
- •Retained FB
- •Radiologic Findings
- •Bronchoscopy
- •Airway Management
- •Rigid Vs. Flexible Bronchoscopy
- •Retrieval Procedure
- •Instruments
- •Grasping Forceps
- •Baskets
- •Balloons
- •Suction Instruments
- •Ablative Therapies
- •Cryotherapy
- •Laser Therapy
- •Electrocautery and APC
- •Surgical Management
- •Complications
- •Bleeding and Hemoptysis
- •Distal Airway Impaction
- •Iron Pill Aspiration
- •Follow-Up and Sequelae
- •Conclusion
- •References
- •Vascular Origin of Hemoptysis
- •History and Historical Perspective
- •Diagnostic Bronchoscopy
- •Therapeutic Bronchoscopy
- •General Measures
- •Therapeutic Bronchoscopy
- •Evidence-Based Review
- •Summary
- •Recommendations
- •References
- •History
- •“The Glottiscope” (1807)
- •“The Esophagoscope” (1895)
- •The Rigid Bronchoscope (1897–)
- •The Flexible Bronchoscope (1968–)
- •Transbronchial Lung Biopsy (1972) (Fig. 42.7)
- •Laser Therapy (1981–)
- •Endobronchial Stents (1990–)
- •Electromagnetic Navigation (2003–)
- •Bronchial Thermoplasty (2006–)
- •Endobronchial Microwave Therapy (2004–)
- •American Association for Bronchology and Interventional Pulmonology (AABIP) and Journal of Bronchology and Interventional Pulmonology (JOBIP) (1992–)
- •References
- •Index

Rigid Broncoscopy |
4 |
|
|
José Pablo Díaz-Jiménez and Alicia N. Rodríguez |
|
Introduction andHistory
Bronchoscopy is the invasive procedure most commonly indicated to diagnose and treat pulmonary problems. There are two kinds of bronchoscopes: the exible bronchoscope (FB), and the rigid bronchoscope (RB). The frst one is the most utilized in clinical practice. However, the rigid bronchoscope is a very important instrument for the diagnosis and treatment of many pulmonary disorders, and has been applied to the airway for many decades.
The interest in reviewing the airway goes back to 1823, when Horace Green introduced frst a sponge and then a rubber catheter into the bronchi, applying silver nitrate to burn lesions located at the level of the larynx and trachea. Later, Joseph O’Dwyer introduced a tube to release adhesions of the lower airways caused by diphtheria, and he also constructed a thin-walled tube to assist in the removal of foreign bodies.
The frst rigid bronchoscopy was introduced by Gustav Killian (Germany) in 1897, who became the Father of Bronchoscopy, after performing the frst rigid bronchoscopy for
J. P. Díaz-Jiménez (*)
Interventional Pulmonary Department, Hospital Universitari de Bellvitge, Hospitalet de Llobregat, Barcelona, Spain
e-mail: pablodiaz@pablodiaz.org
A. N. Rodríguez
School of Medicine, National University of Mar del Plata, Buenos Aires, Argentina
the extraction of a foreign body (a small piece of a pig bone) in a 63-year-old patient. For the procedure, Killian used an esophagoscope and rigid forceps [1]. Chevalier Jackson, from Philadelphia, Pennsylvania, USA, popularized this new bronchoscopic technique and developed the most widely used rigid bronchoscope at the time. His idea of placing a small light in the distal part of the endoscope revolutionized the endoscopist’s ability to examine the airways. In 1916, he established bronchoesophagology departments in fve hospitals in Philadelphia, training many well-known bronchoesophagology professionals [2, 3].
During more than 70 years, the rigid bronchoscope or open tube was the only available instrument to review the airway. At frst, it was mainly used to remove foreign bodies or dilate strictures, but later new applications were described: aspiration of secretions, hemoptysis treatment, biopsies, etc.
Shigeto Ikeda’s exible bronchoscope (FB) development in the 1960s [4] has been the most signifcant advance in the area of bronchoscopy, and has changed the practice to our days, allowing the pulmonology physicians to develop ability in performing exible bronchoscopy and also gave place to the introduction of new technologies specifcally designed to apply with FB.
Shortly after its invention, the FB almost replaced the RB in clinical practice. However, the rigid bronchoscope is still a very important
© The Author(s), under exclusive license to Springer Nature Switzerland AG 2023 |
51 |
J. P. Díaz-Jiménez, A. N. Rodríguez (eds.), Interventions in Pulmonary Medicine, https://doi.org/10.1007/978-3-031-22610-6_4

52 |
J. P. Díaz-Jiménez and A. N. Rodríguez |
|
|
instrument in the study and treatment of airway disorders.
Rigid and exible bronchoscopes complement each other in many indications, and there is no reason to see their application in opposite terms, since each instrument has strengths and limitations. In this chapter, we will review our experience on RB, along with a complete discussion on indications and contraindications.
cult. The RB, in turn, allows the patient to breathe through it, favoring spontaneous breathing and mechanical ventilation while performing the procedure.
The rigid bronchoscope has undergone modifcations over time, particularly after laser resection and stent placement became regular indications for different airway conditions. The most used brand names today are Efer(R), Storz(R), and Wolf® and Novatech.
Overview ofRB
The RB is a stainless steel open tube with variable lengths and widths. It has a distal end, beveled and smooth, and a proximal end that can be adapted to a metallic universal head with several side ports. The distal end is used to lift the epiglottis during intubation, and is also very useful to dilate strictures and to “core” tumors. Lateral openings or fenestrations are present to allow contralateral lung ventilation while working.
The RB is the preferred instrument for endoscopic resections. The rigid tube is the only device that allows a complete control on the airway, assuring proper oxygenation and ventilation while performing, for instance, a laser resection. Aspiration of blood, secretions, and smoke can be easily achieved at the same time that an excellent view of the central airway is depicted.
One of its main strengths is the ability to confront serious hemorrhagic accidents, or airway obstruction from various etiologies: benign or malignant conditions, foreign bodies, mucus plugs, etc. Although unusual, massive hemorrhages can occur even in routine fber bronchoscopies. The RB allows the application of pressure on the hemorrhagic area until hemostasis occurs, giving suffcient time to apply other therapeutic modalities, which can bring a defnitive solution to the problem. It is also particularly useful in the pediatric population. Children’s airway diameter is very small, and it is preferable to use a hollow tube in order to allow spontaneous breathing or assisted ventilation. The FB blocks the airway, and the patient has to breathe around it, increasing signifcantly the airway resistance and work of breathing, making the procedure more diff-
Innovations
The frst rigid bronchoscope for laser application was designed by Jean François Dumon (Fig. 4.1), from Marseille, France, for the brand Wolf. In contrast to other rigid bronchoscopes, the Wolf system has two lateral ports (one for the laser fber and the other one for the suction catheter) and a rotating ventilation connector that allows assisted ventilation without interrupting the treatment. All ports can be occluded to allow closed
Fig. 4.1 Dr. J.F. Dumon
Данная книга находится в списке для перевода на русский язык сайта https://meduniver.com/

4 Rigid Broncoscopy |
53 |
|
|
circuit ventilation. Based on this experience, the Dumon-Harrel (Efer) universal rigid bronchoscope was later developed. It associated modifcations already present in the Wolf system with other advantages, such as the possibility of using a series of 11 interchangeable tubes with increasing diameters available in 2 different lengths: the short tubes (Fig. 4.2) for endotracheal treatments, with no side orifces (diminishing the air lost in the trachea); and the long tubes for endobronchial treatments, with lateral orifces that allow an adequate ventilation even when the bronchoscope
is placed in a peripheral bronchus. Internal and external diameters are color coded on each tube (from 3.5 to 10 mm internal diameter and from 4 to 12 mm external diameter). Available tubes for pediatric use have an internal diameter from 3 to 5 mm and are 20 cm in length.
The head of the rigid bronchoscope can be adapted to the desired tube, according to the different needs (Figs. 4.3 and 4.4).
Fig. 4.4 Rigid bronchoscope with ancillary tools and connection for ventilation
Fig. 4.2 Dumon’s rigid bronchoscope
Fig. 4.3 Universal head of the rigid bronchoscope
Fig. 4.5 Rigid telescope (optic)
The Dumon-Harrel rigid bronchoscope comes with a separate deployment system for the silicone (Dumon) prosthesis.
Another Dumon-Harrel system innovation is the fact that it is possible to lift the superior part of the lateral door, allowing the aspiration of large tumor fragments without modifying the position of the suction catheter. The securing caps are made of silastic, with one or several orifces of different sizes. These caps are much more solid than the usual rubber ones, allowing a more hermetic closure, optimizing ventilation.
The rigid optics offer direct 0° vision (Fig. 4.5); they come in three diameters, 3.5, 5.5, and 7 mm, and they are not fxed. There is also a smaller optics for pediatric use. These instruments easily slide through the silastic caps, and can be moved back and forth according to need. It is a very useful feature to avoid sudden move-
54 |
J. P. Díaz-Jiménez and A. N. Rodríguez |
|
|
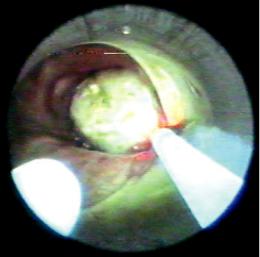
Fig. 4.6 Correct position of the suction catheter and laser fber into the rigid bronchoscope (RB). It is important to always see the tip of the bronchoscope during the procedure
ments that can injure the airway. The rigid optic can be pulled back to avoid midst, or loss of visualization due to blood or detritus. The rigid optic, suction catheter, and laser fber are independent inside the rigid tube, making handling easier.
The most comfortable position when applying laser is placing the tip of the laser fber advanced within the airway, the suction catheter located slightly back to the laser tip, and the rigid optic further back from the working feld (Fig. 4.6). The independence of these elements allows modifying at any time their position according to the intervention needs.
The RB has been designed to present a universal character; in other words, to adapt to multiple endoscopic situations. In addition to laser application settings described above, this instrument can take other confgurations: all or some of the entrance ports can be used (from one to three), open or closed ventilation circuit (for “jet ventilation,” manually assisted ventilation, or spontaneous ventilation), use of short or long tubes, adult or pediatric tubes, and allowing diagnostic and/or therapeutic procedures on practically any group of patients.
Thinking that the rigid bronchoscopy technique had to be simplifed in order to be more
easily used among the interventional bronchoscopy community, H. Dutau, from J.F. Dumon’s team in Marseille, developed a new RB system in collaboration with Karl Storz (manufacturer) and Novatech (distributor): the Dutau-Novatech Rigid Bronchoscope (DNRB) (Fig. 4.7). This new model is more simple to use and it adapts better to new technologies and facilitates the association with FB.
Among the new features that this system provides, one can list: a snap ft connection of the tubes to the head allowing easier attachment and detachment; an iso-connection of the tubes (once the head has been detached) to the ventilation circuit, which improves ventilation while preventing air leak when spontaneous ventilation is used during general ventilation—this iso-connection allows an easier utilization of the FB (Fig. 4.8); a smaller detachable head allowing easier handling (Fig. 4.9); and a 45° angled bevel tip of the tubes, which are less traumatic without reducing the possibility to core out endoluminal lesions. Graduations on the outer surface of the tubes allow measurements of lesions and facilitate stent dimension decision.
The complete DNRB adult set will include 3 tracheal tubes (14, 13, and 12 outer diameter) and 5 bronchial tubes (14, 13, 12, 11, and 9 outer diameter), a detachable head including the body’s head, the ventilation connector, and a 3-divided detachable side port including 1 channel for the suction, 1 for exible probes (such as laser, electrocautery, or cryotherapy probes), and 1 for the jet ventilation connection (Fig. 4.7).
The DNRB is compatible with all the Karl Storz rigid instruments and with the Tonn silicone stent loading and insertion system.
The variant of Storz rigid bronchoscope for laser bronchoscopy was designed by Shapshay from Boston, USA. It is specially manufactured for jet ventilation, and for this reason it has a fxed port designed to serve this purpose. It is available in 10 mm internal diameter size (12 mm external diameter), presenting also a connection for ventilation and two additional ports [5].
A recently introduced rigid bronchoscope, called Rigid Integrated Bronchoscope developed by Wolf, presents separate channels for optics
Данная книга находится в списке для перевода на русский язык сайта https://meduniver.com/

4 Rigid Broncoscopy |
55 |
|
|
Fig. 4.7 The Dutau-Novatech Rigid Bronchoscope (DNRB)
Fig. 4.8 An iso-connection of the tubes (once the head has been detached) to the ventilation circuit, which improves ventilation while preventing air leak when spontaneous ventilation is used during general ventilation. This iso-connection allows an easier utilization of theexible bronchoscope (FB)
and instruments, and integrates the operator head with the camera. It has also an irrigation port to wash the distal lens. It has the advantage of increasing the working space and thus
Fig. 4.9 A smaller detachable head allowing easier handling
improves manipulation within the bronchoscope. However, the vision is limited since the camera does not go further distal to the end of the rigid bronchoscope.
It is clear that the RB, although keeping its original basic shape, has suffered several modifcations to adapt to specialized procedures,
