
- •NEONATAL DERMATOSIS
- •OUTLINE
- •SKIN FUNCTION IN THE NEONATE
- •ECCRINE SWEATING
- •SEBACEOUS GLAND SECRETION
- •PREVELANCE OF NEONATAL DERMATOSIS
- ••Cutaneous manifestations were observed in 90.5% of the newborns.
- ••With respect to mode of delivery, Vaginally delivered neonates showed significant association with
- •TRANSIENT PHYSIOLOGICAL CHANGES
- •VERNIX CASEOSA
- ••Golden yellow staining - Haemolytic disease of the newborn and postmaturity.
- •FUNCTIONS
- •PERIPHERAL CYANOSIS/ ACROCYANOSIS
- ••The cyanotic hue disappears on warming the extremities.
- •HARLEQUIN COLOUR CHANGE
- ••Wide variation in the duration of attacks, but generally between 30 seconds- 20
- ••As skin matures, this vascular phenomena disappears.
- •CUTIS MARMORATA
- •MONGOLIAN SPOT
- ••Cause-arrested embryonal migration of melanocytes from neural crest to epidermis resulting in dermal
- ••Lesions also occur on the buttocks, dorsal trunk and extremities.
- •SEBACEOUS GLAND HYPERPLASIA
- •SEBACEOUS GLAND HYPERPLASIA
- •MILIA
- •MILIA
- •PALATE-EPSTEIN’S PEARL
- •DESQUAMATION (PHYSIOLOGICAL SCALING OF
- •MACULAR HEMANGIOMA
- •MINIATURE PUBERTY
- ••Scrotal hyperpigmentation and labial hypertrophy-most common findings in miniature puberty .
- ••Enlargement of breast tissue with thick milk-like secretion (witch’s milk) may be seen.
- •SUCKING BLISTERS
- •NEONATAL OCCIPITAL ALOPECIA
- ••The roots in the occipital area do not enter telogen until term, therefore
- •NEONATAL ACNE/ NEONATAL CEPHALIC
- •No additional treatment is needed -usually resolves spontaneously within four months without scarring.
- •LANUGO
- •ANETODERMA OF PREMATURITY
- ••It is non progressive and persistent.
- •SKIN DISORDERS IN THE NEONATE
- •ERYTHEMA TOXICUM NEONATORUM
- ••Commonly seen-term infants, rare in preterm and low birth weight infants.
- ••Could be an innate immune response of a newborn infant to commensal microbes
- •Diagnosis :
- •TRANSIENT NEONATAL PUSTULAR MELANOSIS
- ••It is transient, benign, self-limiting dermatoses of unknown aetiology characterised by 3 types
- •One hour after birth, flaccid vesiculopustules and superficial erosions with minimal surrounding erythema
- •MILIARIA
- ••Miliaria rubra and miliaria crystallina-common in neonates.
- •MILIARIA CRYSTALLINA
- ••Delicate and generally rupture within 24 hr, and are followed by bran-like desquamation.
- •MILIARIA RUBRA (‘PRICKLY HEAT’)
- ••Lesions occur in -flexural areas, especially around the neck and in the groins
- ••Frequently, some lesions are pustular (miliaria pustulosa), but this does not necessarily indicate
- •Management
- •DIAPER DERMATITIS (NAPKIN DERMATITIS OR
- •Three common types of diaper dermatitis are are -
- •Treatment :
- •APLASIA CUTIS CONGENITA
- ••Aplasia cutis congenita may be associated with under lying embryologic malformations like
- •BACTERIAL INFECTIONS
- ••Common skin problems seen in neonates in India.
- •IMPETIGO
- ••Varnish coloured crust is seen.
- •When bullae spread, rupture, and involve large areas, infection may spread systemically, causing
- •DIAGNOSIS :
- •STAPHYLOCOCCAL SCALDED SKIN SYNDROME(SSSS)
- ••The site of blister cleavage is the granular layer.
- ••The first sign of the disease - faint, macular, orange red, scarlatiniform eruption
- •TREATMENT :
- •OMPHALITIS
- •ECTHYMA GANGRENOSUM
- ••Predisposing factors- prematurity, renal failure, neutropenia and immunodeficiencies, necrotizing enterocolitis and bowel surgery.
- •VIRAL INFECTIONS
- •NEONATAL HERPES SIMPLEX
- ••The skin lesions appear between days 2 and 20.
- ••During an intrauterine infection, vesicles appear within 1 day of life.
- •Neonatal herpes simplex showing congenital ulceration and scarring at 10 days.
- •DIAGNOSIS
- •FETAL VARICELLA SYNDROME
- •Pregnant women who are not immune (on the basis of history, and, preferably,
- •FUNGAL INFECTIONS
- •NEONATAL CANDIDIASIS
- ••White, “flaky,” creamy patches are seen on the tongue and mucous membranes of
- ••In the surrounding normal skin there may be punctate erythematous lesions, sometimes pustular
- •CONGENITAL CANDIDIASIS
- ••Palmar and plantar pustules are regarded as a hallmark of congenital cutaneous candidiasis
- •Congenital candidiasis in a neonate born at 24 weeks’ gestation. Note the “burn-like”
- •DISORDERS CAUSED BY TRANSPLACENTAL
- •NEONATAL PEMPHIGUS VULGARIS
- ••No treatment is required as the lesions have resolved spontaneously within about 3
- •NEONATAL LUPUS ERYTHEMATOSUS
- ••It occurs in neonates up to 3 months old.
- ••A ‘spectacle like’ distribution of lesions around the eyes is especially characteristic.
- •Pathology
- ••Infants generally show little sign of residual disease after the age of 1
- •GENODERMATOSIS
- •SOURCE-IADVL
- •MISCELLANEOUS DISORDERS
- •COLLODION BABY
- ••Almost 90% of collodion babies will go on to develop a severe form
- ••Within hours, this membrane
- •MANAGEMENT
- •REFERENCES

NEONATAL DERMATOSIS
PRESENTED BY
Dr. Ashwajit Singh1

OUTLINE
•SKIN FUNCTION IN THE NEONATE
•PREVELANCE OF NEONATAL DERMATOSIS
•TRANSIENT PHYSIOLOGICAL CHANGES
•SKIN DISORDERS IN THE NEONATE
•BACTERIAL INFECTIONS
•VIRAL INFECTIONS
•FUNGAL INFECTION
•MISCELLANEOUS DISORDERS
2
SKIN FUNCTION IN THE NEONATE
•Normal full term infant-functional stratum corneum & fully developed barrier function.
•TEWL(transepidermal water loss)- higher in the first few days of life but rapidly improves.
3
•Impaired barrier function-preterm neonate, especially <34 weeks gestation.
•Barrier function- improves rapidly after birth in the preterm infant-normal by the end of the 2/3rd week after birth.
4

ECCRINE SWEATING
•Anatomically normal eccrine sweat gland-28th week of gestation
•Functionally immature in neonates born <36 weeks of gestation.
•Response usually develops in such babies by 2 weeks after birth.
5

•Neonates born >36 weeks of gestation sweat in response to thermal stress from birth.
•The forehead -principal site of thermally induced sweating in the neonate.
6

SEBACEOUS GLAND SECRETION
•Sebum secretion rates-high in neonates
•Stimulation of sebaceous gland activity- androgen, Dehydroepiandrosterone.
•Secretions of the fetal sebaceous glands- significant contribution to the vernix caseosa.
•Sebaceous gland activity decreases -about the end of the first month to reach a stable level by the end of the first year.
7
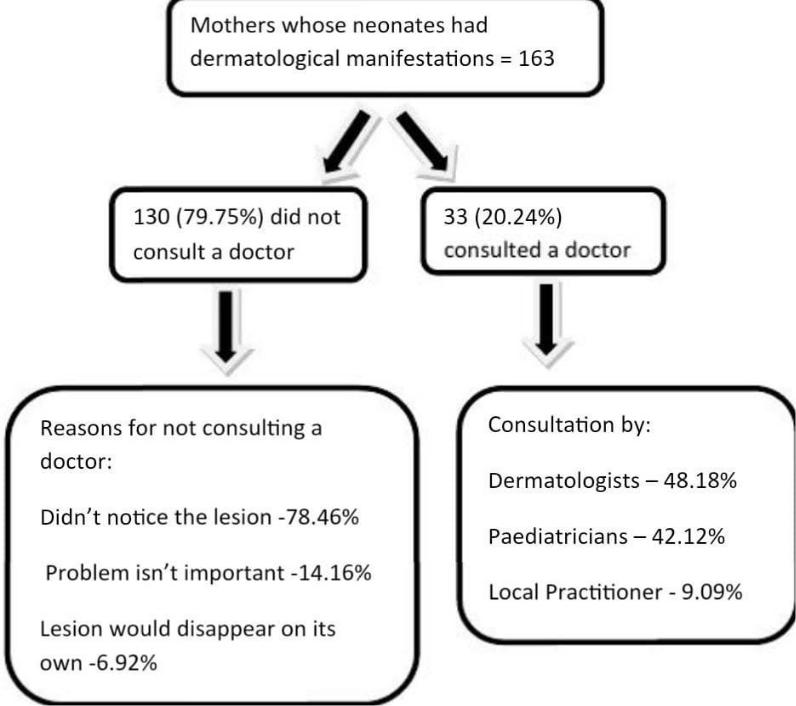
PREVELANCE OF NEONATAL DERMATOSIS
•A cross sectional descriptive study was conducted from October 2011 to August 2013 at JSS Hospital, Mysore, involving 180 neonates and their mothers.
•Neonates were examined for cutaneous manifestations and the other variables that were analyzed are newborn sex, mode of delivery, birth weight, gestational age, and no. of pregnancies.
8
•Cutaneous manifestations were observed in 90.5% of the newborns.
•Majority (77.2%) had physiological skin changes.
•Pathological skin changes were significantly higher in newborns delivered to primi, para and low birth weight neonates.
•Most common skin changes seen were milia, mongolian spots, physiological desquamation, epstein pearls, erythema neonatorum, miliaria.
9
•With respect to mode of delivery, Vaginally delivered neonates showed significant association with occurrence of Milia, Epstein pearls, Physiological desquamation and Physiological hypertrichosis lanuginosa
•Neonates delivered by Caesarean section showed significant association with Erythema neonatorum and Miliaria (p<0.05).
10
11
