
- •LIVER DISEASES
- •LIVER DISEASES
- •Do you know that …
- •Liver structure v. portae system
- •Liver
- •Liver functions
- •Major risk factors for liver disease
- •Symptoms of liver disorders
- •Fatigue
- •Jaundice
- •Jaundice or icterus
- •Jaundice: major types
- •Causes of jaundice
- •Darkening of the Urine
- •Pale (light) Stools
- •Liver Pain
- •Ascites
- •Ascites, umbilical hernia
- •Ascites
- •Симптомы и синдромы заболеваний печени
- •ПОРТАЛЬНАЯ ГИПЕРТЕНЗИЯ
- •Possible levels of block in portal hypertension
- •Hepatocellular cytolisis
- •Stigmata of chronic liver disease
- •Cholestasis syndrom
- •CHOLESTASIS
- •Etiology of Dupuitren contracture
- •Etiologic factors of gynecomastia
- •polyneuropathia
- •ПРИЧИНЫ ПОРТАЛЬНОЙ ГИПЕРТЕНЗИИ
- •Расширенные вены передней стенки живота, асцит
- •ЭГДС.
- •Расширение v. рortae и vv. hepaticae
- •ПЕЧЕНОЧНОКЛЕТОЧНАЯ
- •ПРИЧИНЫ ПЕЧЕНОЧНОЙ НЕДОСТАТОЧНОСТИ
- •Синдром печеночно-клеточной недостаточности
- •Печеночная энцефалопатия
- •ГЕПАТОРЕНАЛЬНЫЙ СИНДРОМ I и II тип
- •Патогенеза гепаторенального синдрома
- •Типы гепаторенального синдрома
- •ФАКТОРЫ, ПРОВОЦИРУЮЩИЕ РАЗВИТИЕ ГЕПАТОРЕНАЛЬНОГО СИНДРОМА (на фоне поражения печени)
- •Желтуха, ксантелазмы
- •ГИПЕРСПЛЕНИЗМ
- •Маркеры хронической алкогольной интоксикации
- •Классификация тяжести поражения печени по Чайлд-Пью
- •ЭГДС – расширенные вены пищевода
- •Пункционная биопсия печени под контролем УЗИ (цирроз)
- •Мелкоочаговое поражение печени при остром гепатите
- •Асцит, расширенная v.portae, неровность контуров при циррозе печени
- •Сцинтиграфия печени с метастазами
- •Сцинтиграфия мелкоузлового цирроза
- •Лапароскопия – крупноузловой цирроз
- •Передняя стенка живота при синдроме портальной гипертензии
- •Компьютерная томография
- •FibroScan®
- •Выраженность фиброза при фибросканировании печени
- •Stages of Liver Disease
- •Progression of Hepatitis B Infection
- •Healthy Liver
- •Healthy Liver
- •Types of Hepatitis
- •Hepatitis B is a Devastating Global Healthcare Issue
- •Hepatitis – Disease Terminology
- •How Hepatitis B is Acquired?
- •How the Infection is Acquired in the West?
- •Hepatitis B – Diagnosis Terminology
- •Diagnosis of Chronic Hepatitis B
- •Signs and Symptoms of HBV Infection
- •Universal Hepatitis B Vaccination
- •Global Control of Hepatitis B
- •Types of viral Hepatitis
- •Healthy Liver
- •Liver biopsy
- •Detection of serologic markers of hepatitis B virus (HBV) infection, as a function
- •Lamivudine is a Potent Inhibitor of HBV Replication
- •Lamivudine has an Excellent Pharmacokinetic Profile
- •Patient Entry Criteria
- •One Year of Lamivudine - Conclusions
- •Resistance to Anti-Viral Drugs
- •Prevention of Hepatitis B
- •Universal Hepatitis B Vaccination
- •Recommendations for Pre-exposure Vaccination
- •Recommendations for Post-exposure Vaccination
- •Global Control of Hepatitis B
- •Concurrent immunologic diseases in type 2 autoimmune hepatitis.
- •Probabilities of clinical, biochemical, and histologic remission during corticosteroid therapy.
- •Clinical features of type 2 autoimmune hepatitis.
- •Liver transplantation for autoimmune hepatitis.
- •Survival expectations and probability of developing cirrhosis during and after corticosteroid treatment.
- •liver biopsy
- •Detection of serologic markers of hepatitis B virus (HBV) infection, as a function
- •The Efficacy and Safety of Lamivudine in HBeAg-positive Chronic Hepatitis B
- •Lamivudine is a Potent Inhibitor of HBV Replication
- •Lamivudine has an Excellent Pharmacokinetic Profile
- •What Patient Populations Have Been Studied
- •Key Lamivudine Clinical Studies (1)
- •Key Lamivudine Clinical Studies (2)
- •Patient Entry Criteria
- •Lamivudine Rapidly Suppresses
- •One Year of Lamivudine - Conclusions
- •Resistance to Anti-Viral Drugs
- •Concurrent immunologic diseases in type 1 autoimmune hepatitis.
- •Probabilities of clinical, biochemical, and histologic remission during corticosteroid therapy.
- •Clinical features of type 2 autoimmune hepatitis.
- •Liver transplantation for autoimmune hepatitis.
- •Survival expectations and probability of developing cirrhosis during and after corticosteroid treatment.
- •ALCOHOLIC LIVER DISEASE
- •Principal alcohol-induced hepatic lesions
- •Alcohol-induced hepatic lesions
- •Pathogenesis of liver injury secondary to chronic ethanol ingestion
- •Equivalents of pure alcohol
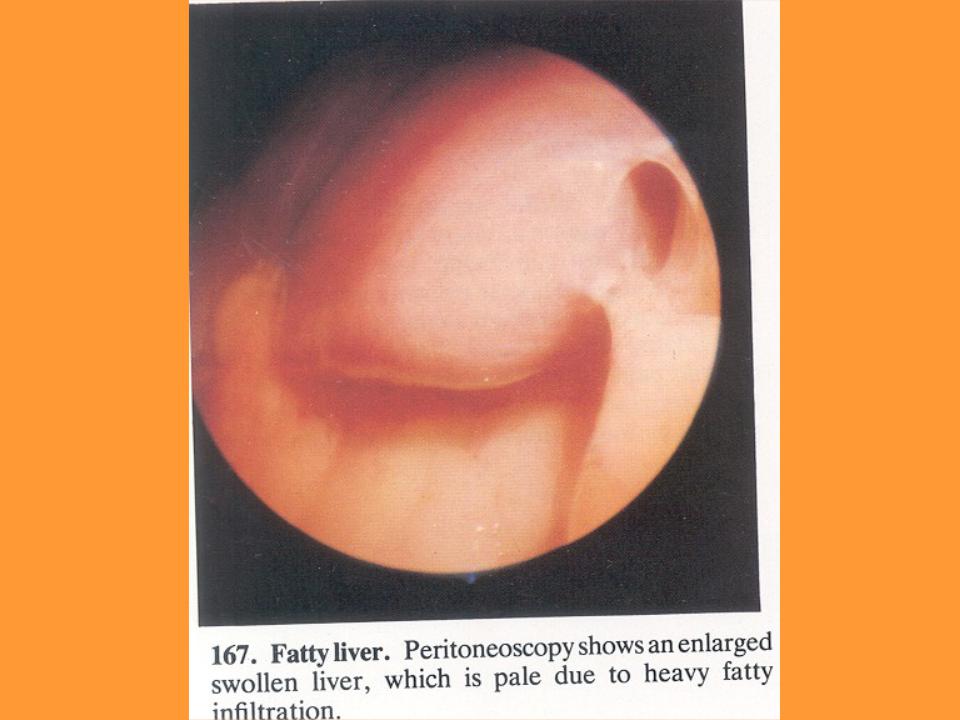
- •Alcoholic fatty liver
- •Two-Hit Model of the Progression of Fatty Liver Disease
- •Alcoholic fatty liver
- •Similarities between Alcoholic and Nonalcoholic Fatty Liver Diseases
- •Alcoholic hepatitis
- •This figure depicts a laparoscopic view of a patient with chronic active hepatitis
- •Percutaneous liver biopsy with or without ultrasonic guidance
- •Alcoholic hepatitis: liver biopsy
- •Treatment of severe alcoholic hepatitis
- •Причины смерти при алкогольном гепатите
- •Alcoholic cirrhosis
- •Alcoholic cirrhosis
- •Alcoholic cirrhosis: clinical manifestations

Alcohol-induced hepatic lesions
• only a minority of consistently heavy drinkers with hepatic steatosis (15 to 20 %) ever have clinically important liver disease (LD)
•Risk factors for serious liver damage in habitual alcohol drinkers include certain polymorphisms in alcohol- metabolizing enzymes, obesity, exposure to other hepatotoxins (e.g., acetaminophen), and infection with hepatitis C
•In many patients, a specific RF is never identified.

Pathogenesis of liver injury secondary to chronic ethanol ingestion
•MAA, malondialdehyde-acetaldehyde
•TNF-a, tumor necrosis factor a
•TGF-b, transforming growth factor b; IL, interleukin

Equivalents of pure alcohol
• |
Strong drinks |
28 ml |
10 g |
• |
Vine |
85 ml |
10 g |
• |
Beer |
230 ml |
10 g |
• |
Minimal dose |
|
|
that cause liver damage - 30 g/day
• 210 g ethanol per week is safe ?

Alcoholic fatty liver
•Clinical manifestations are often minimal or entirely absent
•the disorder may not be recognized unless another illness (frequently alcohol-related) brings the patient to medical attention
•Hepatomegaly, at times accompanied by tenderness, may be the only finding
•Jaundice, ascites, and edema are seen only with more serious liver injury.

Two-Hit Model of the Progression of Fatty Liver Disease
•The earliest stages of FLD involve exposure of hepatocytes to TNF-a
•TNF-a initiates various intracellular signals mitochondrial permeability and the release of reactive oxygen species (ROS).
•Left unchecked, these responses promote hepatocyte apoptosis.
•Most healthy hepatocytes use some of the potentially lethal signals (e.g.,ROS) to activate a multifaceted response that permits
the hepatocytes to survive.
•Secondary insults (second hits) that inhibit this adaptation also result in apoptosis
•Even when adaptation is successful and hepatocytes remain viable, they become extremely vulnerable to other insults that partially depolarize the mitochondrial inner membrane, dying by necrosis when the mitochondrial membrane potential collapses.

Alcoholic fatty liver
•Fatty liver invariably develops after heavy alcohol intake
•It can progress to alcoholic hepatitis and cirrhosis
•In some patients, alcoholic hepatitis is a necessary step in the development of alcohol-induced cirrhosis
•However, in some other patients alcohol may stimulate the production of fibrosis and cirrhosis without requiring alcoholic hepatitis as an intermediate lesion.

Similarities between Alcoholic and Nonalcoholic Fatty Liver Diseases
• |
Obesity (OB) and alcohol abuse (AA) are associated with the |
same |
spectrum of |
|
liver diseases. |
|
|
|
|
• |
The time course for the progression of disease and the RR of |
cirrhosis are also |
||
similar in obesity-related liver disease |
(ORLD)and ARLD |
|
|
|
• |
Distinct, but mutually enhancing, mechanisms may also be |
involved |
|
|
• |
The similar pathologic features and natural histories of the two |
types of |
||
FLD suggest that common pathogenic mechanisms may be involved. |
|
|||
• |
A fatty liver is more common in pts with OB and AA than in those with either |
|||
alone. |
|
|
|
|
• |
Moreover, OB is an independent RF for cirrhosis in pts who AA Thus, elucidation |
|||
of the mechanisms that cause ORLD is |
liikely to clarify the role of pluripotent |
|||
cytokines, such as TNF- a , in promoting alcohol-induced liver damage.

Alcoholic hepatitis
• The clinical features AH resemble those of viral or toxic liver injury
–anorexia, nausea and vomiting, malaise, weight loss, abdominal distress, and jaundice
–Fever is seen in about half of cases.
•On physical examination
–tender hepatomegaly is common
–splenomegaly is found in about one-third of patients
–the patient may have cutaneous arterial "spider" angiomas and jaundice
More severe cases may be complicated by ascites, edema, bleeding, and encephalopathy.

This figure depicts a laparoscopic view of a patient with chronic active hepatitis and early cirrhosis

